Shoulder:The Shoulder in Athletes
Contents
- 1 Bullet points
- 2 Key words
- 3 Thrower’s Shoulder
- 3.1 Introduction
- 3.2 Theories and controversies in the last 30 years explaining pain and pathogenesis
- 3.2.1 Anterior subacromial impingement theory
- 3.2.2 Microinstablity theory
- 3.2.3 Theory of microtrauma caused by repetitive biceps traction
- 3.2.4 Theory of trauma by compression or distraction
- 3.2.5 Mechanical impingement theory: posterosuperior glenoid impingement or “internal impingement”
- 3.2.6 Hyperabduction theory
- 3.2.7 Functional theory
- 3.3 Suprascapular neuropathy in repetitive overhead athletes
- 3.4 Long thoracic nerve injury in repetitive overhead athletes
- 3.5 Diagnosis
- 3.6 Imaging
- 3.7 Isokinetic assessment
- 3.8 Arthroscopic assessment
- 3.9 Treatment
- 3.9.1 Technopathy and sports technique correction
- 3.9.2 Rehabilitation
- 3.9.3 Surgery
- 3.9.3.1 Arthroscopic debridement
- 3.9.3.2 Arthroscopic arthrolysis
- 3.9.3.3 Postero-superior glenoidplasty
- 3.9.3.4 Arthroscopic repair of superior labral tear from anterior to posterior (SLAP) lesions
- 3.9.3.5 Biceps tenodesis under arthroscopic control
- 3.9.3.6 Arthroscopic rotator cuff repair
- 3.9.3.7 Derotational osteotomy
- 3.10 Conclusion
- 4 Swimmer's Shoulder
- 5 References
Bullet points
- There are four major theories that have been used to explain pathology in the overhead athlete: Frank Jobe's micro-instability theory, Christopher Jobe’s hyperabuction theory, Walch's posterosuperior impingement theory, and Burkhart, Kibler, Morgan’s posterosuperior instability and superior labral tear from anterior to posterior (SLAP) lesion theory.
- Clinical examination must look for stiffness (in internal rotation: glenohumeral internal rotation deficit (GIRD) > 20 degrees), instability, rotator cuff pathology and other more specific SLAP tests: active compression, crank, speed, Dynamic Labral Shear test (O'Driscoll's test).
- The anatomical assessment, ideally using simple radiographs and magnetic resonance arthrography (MRA), may be complemented by an isokinetic functional assessment looking for external rotator imbalance where the external to internal strength ratio is < 66%.
- Treatment is mostly conservative (and ideally preventive), involving a structured rehabilitation program: correction of athletic movements (keeping the elbow forward and avoiding excessive retropulsion to limit internal impingement, compact serve), range of motion recovery by ‘sleeper stretching’, and eccentric external rotator strengthening, ideally in an isokinetic mode.
- The surgical indication must be rational and carefully thought-out because the results are often disappointing for athletes. The idea is not to try to fix everything and to remember that many “findings” are in fact adaptations of the throwing athlete. Thus, it is important that every effort is made to identify the true cause of the pain.
- Surgical treatment is often ‘salvage’ in nature, because even if the published results show improved functional scores, only half of the patients return to the same sports level, whatever technique is used. Surgical treatment of concomitant tears can lead to stiffness, preventing a return to previous athletic performance.
- Full thickness rotator cuff repair often spell the end of a professional sports career.
Key words
Thrower’s shoulder; superior labral tear from anterior to posterior (SLAP) lesions; Labrum repair; Posterosuperior impingement; Arm cocking pain; Dead arm; Glenoplasty; Sleeper stretch; Arthrolysis.
Thrower’s Shoulder
Introduction
The subject of thrower’s shoulder is vague and the term needs elaboration. It is not clear what symptomatologies and pathologies are and to which athletes this term can be applied to. It is not necessarily synonymous with superior labral tear from anterior to posterior (SLAP) tears or posterosuperior impingement.
No doubt athletes will seek help when their performance is constrained by painful symptoms. Secondary phenomena may be involved, such as internal disturbances, cracking, strength loss, ‘dead arm syndrome’ (characterized by discomfort either after arm cocking or at the start of throwing). This discomfort can be more or less debilitating, ranging from a decrease in performance to complete cessation, or even the end of a professional career.
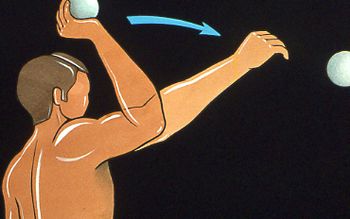
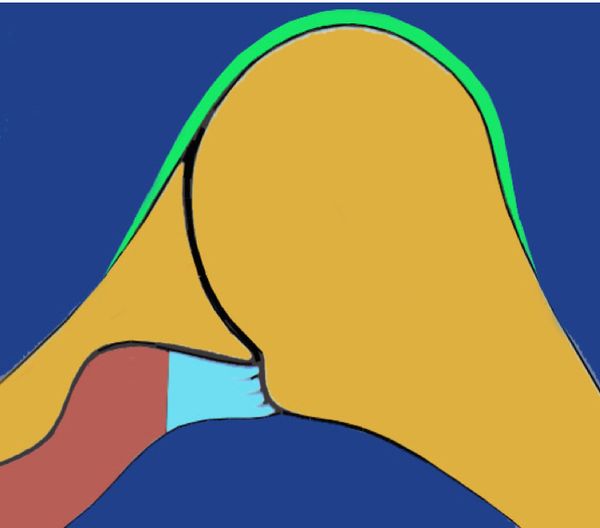
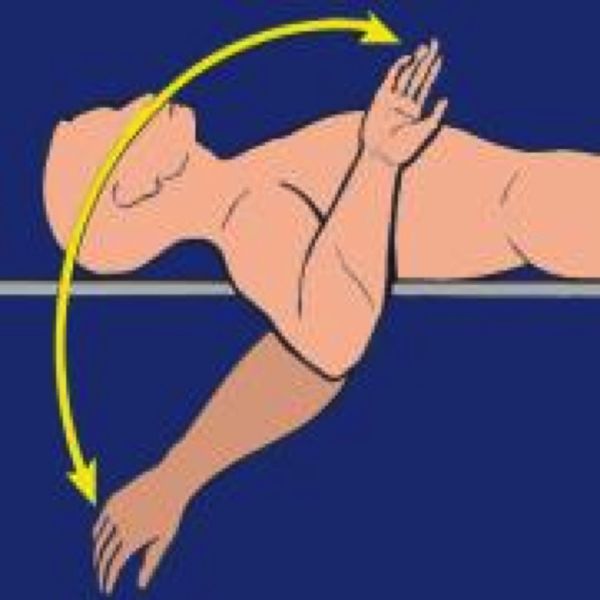
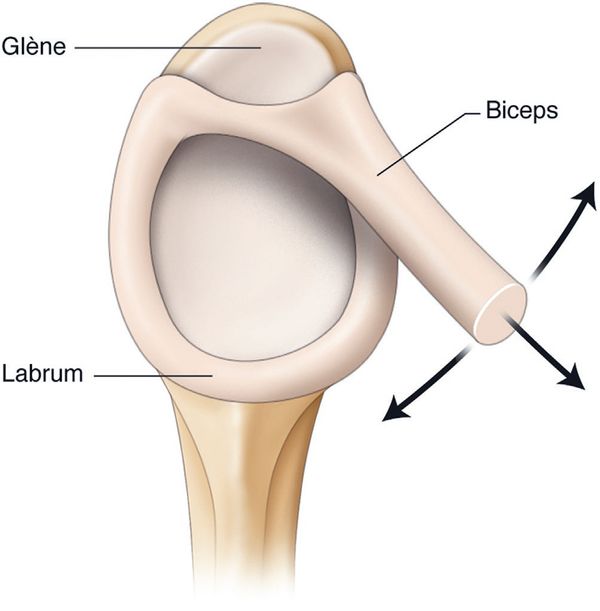
Athletes susceptible to these disorders are also not always strictly throwers, such as baseball pitchers. In fact, a contact component can also occur in tennis, volleyball, handball, water polo or rugby (arm cocking countered by an opponent). Thus, all sports that involve arm cocking can fit into this nosological framework (Figure 1).
As to pathogenesis, too much importance has been attributed to superior labral tear from anterior to posterior (SLAP) lesions to explain these painful shoulders, so a classification of the numerous pathologies is essential to define a therapeutic strategy.
There is not always a consensus between terminologies and theories worldwide. This is probably partly explained by the fact that there is a great cultural diversity between athletes from different countries. In fact, the literature has been flooded with articles evoking the pathologies developed by the baseball pitcher, a favorite sport in North America, while not mentioned at all in Europe, where contact sports like rugby or handball are more prolific. Faced with these very different terminologies and athletes, a practical classification, based on clinical, paraclinical and functional examinations, so as to discuss therapeutic options. Anatomic lesions must be differentiated from non-lesional dysfunction where preventive treatments are of great importance.
Theories and controversies in the last 30 years explaining pain and pathogenesis
Anterior subacromial impingement theory
Neer and co-authors were among the first to propose this theory, but Tibone et al. showed disappointing results for open acromioplasty: only 22% of throwers resumed activity at the same performance level.[2][3]
Microinstablity theory
In 1979, Frank Jobe et al. developed the ‘microinstability’ theory, in which anterior instability was caused by repetitive stretching of the anterior capsuloligamentous structures through repeated arm cocking movements. Although success has been reported in 68% of cases with capsular ligamentous retention procedures, the results of capsular tightening were mediocre.[4]
Theory of microtrauma caused by repetitive biceps traction
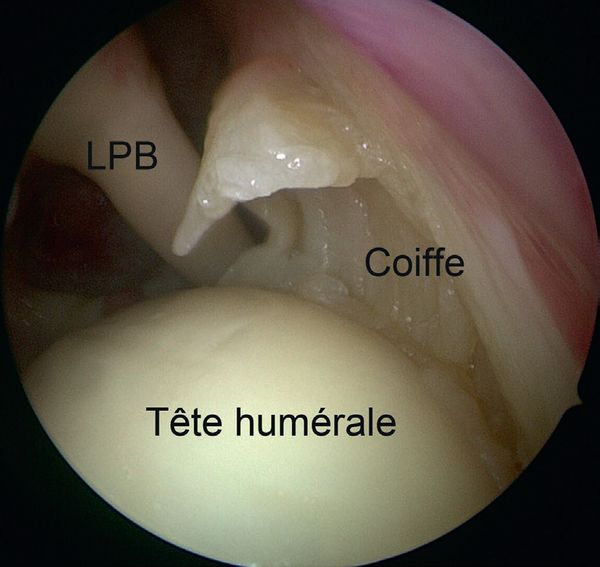
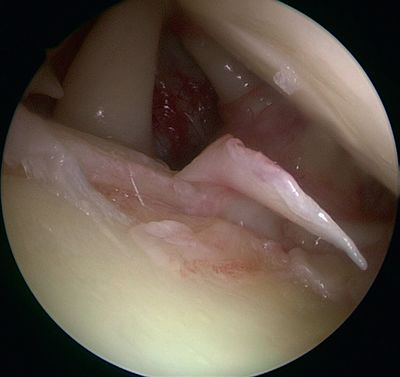
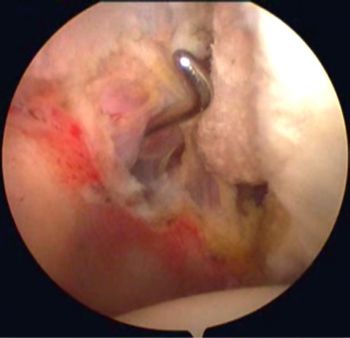
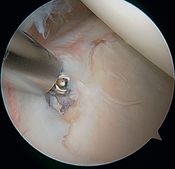
In 1985, Andrews et al. were the first to see superior labral tears under arthroscopy (Figure 3 and Video 1) in 36 throwing athletes (sometimes associated with articular rotator cuff tears, Figure 3).[5]
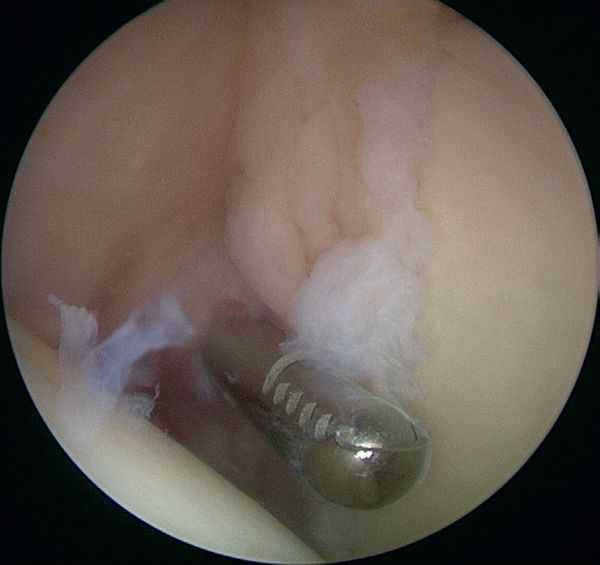
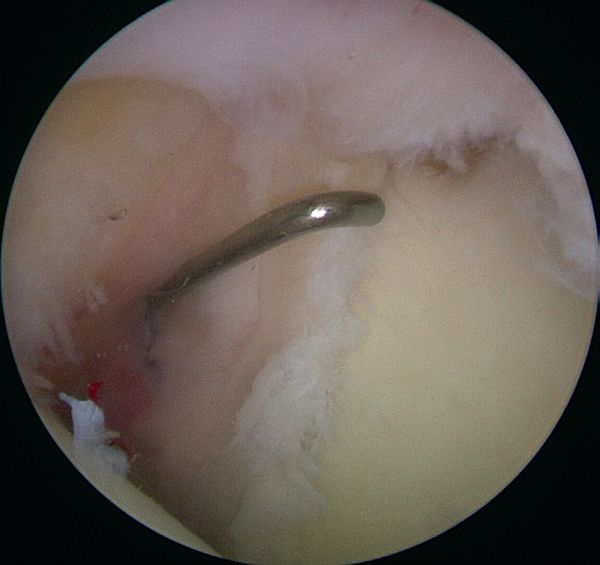
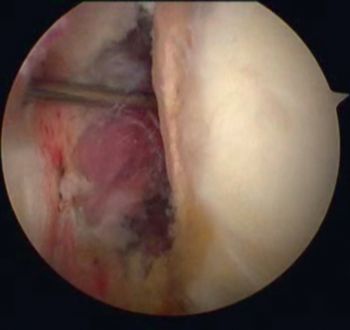
They reported that simple debridement allowed 85% of athletes to resume their sport at the same level (Figure 4 and Video 2).
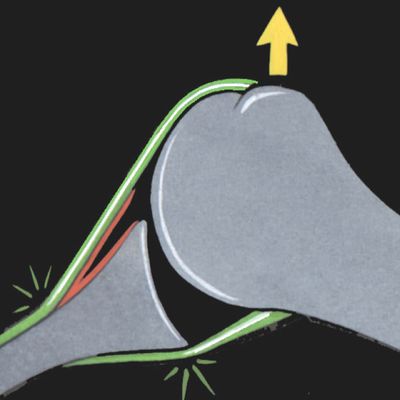
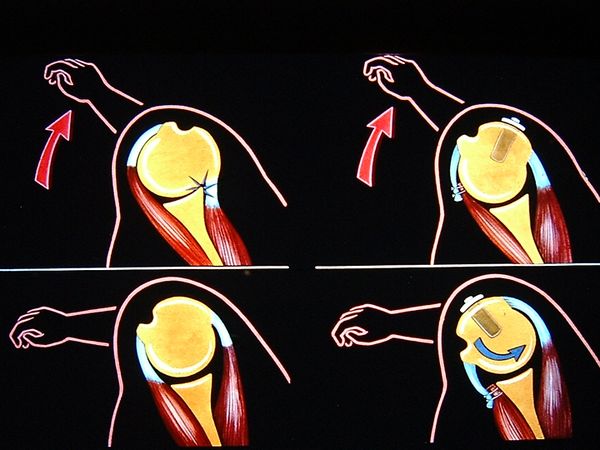
The authors accounted for the labral tears by repeated biceps traction on its labral tendon attachment, progressively disinserting it from the superior glenoid rim (chronic microtrauma, Figure 5).
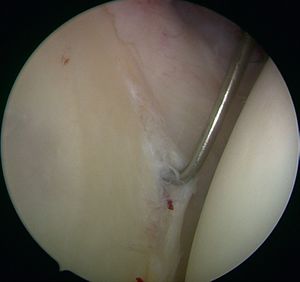
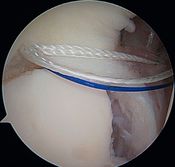
This progressive avulsion is taken-up by Burkhart et al. as the aptly termed ‘peel-back mechanism’ observed by reproducing the cocking phase under arthroscopic control, confirming the medial pivot of the posterosuperior labrum around the posterosuperior glenoid rim (Figure 6 and Video 5).[6]
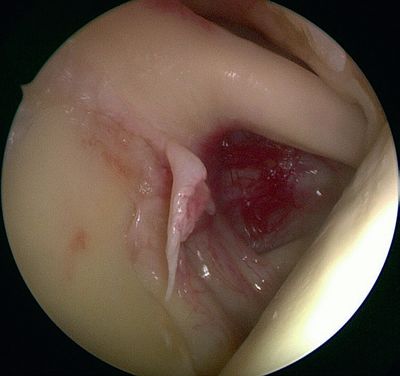 Figure 6A. Arthroscopic view (right shoulder) of a labral tear, elbow at side: before performing the arthroscopic dynamic test when the arm is cocked with retropulsion, and the appearance of Burkhart’s peel-back mechanism. Reproduced with permission from XX.[6] |
Theory of trauma by compression or distraction
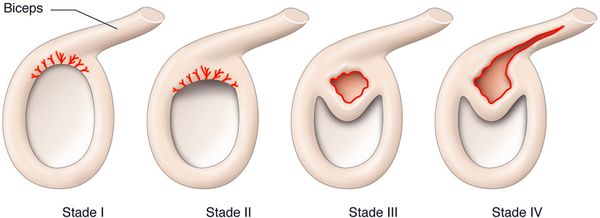
In 1990, Snyder et al. classified superior labral tears, which they defined by the acronym SLAP (superior labral tear from anterior to posterior), still used today (Figure 7).[7]
Snyder’s 4 stage classification of superior labral SLAP lesions
However, it is a retrospective study of 700 arthroscopies, performed between 1985 and 1988, with only 2 throwing athletes out of 27 patients, who had superior labral tear from anterior to posterior (SLAP) lesions (mainly type II, Figure 8, Video 4).
Contrary to the theory of Andrews et al., Snyder et al. believe that the origin is essentially traumatic, according to two mechanisms: a fall stopped by the palm of the hand, arm outstretched (compressive force on the labrum, Figure 9A) or a violent traction with extended arm (distractive force on the biceps and its labral attachment, Figure 10).
Origin of lesion with a compressive force on the labrum
These two tear mechanisms have been confirmed in cadaveric models.[8][9]
Snyder et al. also suggest the possibility of suturing the superior labrobicipital complex by transosseous techniques (anchors or staples) and they described numerous adjuvant pathologies (31% partial and full-thickness rotator cuff tears, 15% instabilities, 15% humeral head lesions, and 11% acromioclavicular arthropathies). Snyder et al, like Jobe et al. proposed that the mechanism is derived from Codman's theory, with a compressive force in posterosuperior translation caused by extension and external rotation of the arm leading to detachment of the labrobicipital complex. Depending on its severity, the trauma can lead to a simple bone contusion on the humeral head, anteroinferior capsular distension, rotator cuff tears, or even worse, to a displaced fracture of the greater tubercle.[10]
Mechanical impingement theory: posterosuperior glenoid impingement or “internal impingement”
Walch et al. developed the theory of isolated posterosuperior impingement by publishing a series of 17 arthroscopies performed in athletes who demonstrated pain in the cocking phase but lacked concomitant instability. They explain this symptomatology by mechanical impingement repeated at 90% of abduction, maximum external rotation and retropulsion (maximum extension), between the greater tubercle and the posterosuperior glenoid rim, causing partial tears in the posterosuperior rotator cuff and the facing glenoid labrum (Figure 10, Videos 5 and 6).[11]
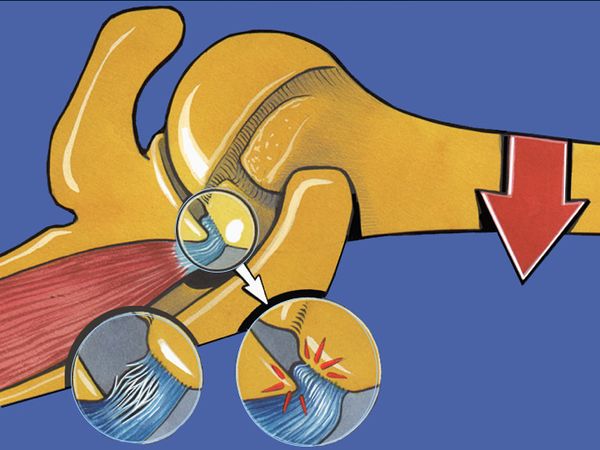
The appeal of this theory is that it is validated by a simple observation when reproducing cocking and retropulsion movements under the arthroscopic control, revealing the tears by repeated contact (Video 7).
They propose treatment by simple debridement, but the results are not as good as those reported by Andrews et al. Sonnery-Cottet et al., in a series of tennis players, reported an 80% return to sport, but only 50% at the same level.[12]
In a series of 75 throwing athletes with posterosuperior glenoid impingement, arthroscopic debridement was disappointing, with a return to the same sports level in only 16% of patients. The authors found 89% partial rotator cuff tears, 90% labral tears (all posterior, except 3), as well as osteochondral tears affecting the glenoid or humeral head. No bicipital tears were found in this series.[13]
Unlike Frank Jobe et al and Burkhart et al., Walch et al. and Lädermann et al. could not confirm any form of micro-instability. Instead, Walch et al. based their argument on the fact that of 1000 instability cases operated, only 10 had concomitant posterosuperior impingement.[14] Using a precise and dynamically in vivo motion analysis of the entire kinematic chain of the shoulder, Lädermann et al. did not observed antero-inferior or static posterosuperior instability.[15]
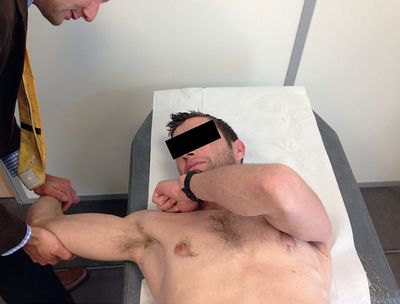
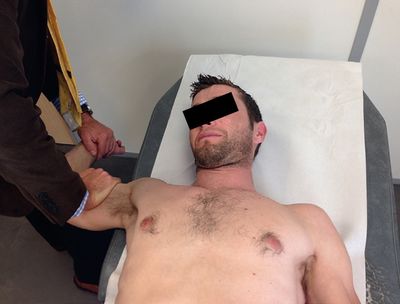
In 1995, Davidson et al. took up this theory and showed how hyper-rotation (hyperabduction) and anterior humeral translation act as the trigger mechanism for pain, and explain how the shoulder relocation test (described by Jobe et al.) reduces the pain by releasing the internal impingement (Figure 11).[16]
Hyperabduction theory
Shoulder relocation test
| A | B |
| Figure 12. Shoulder relocation test. Pain is experienced during cocking (a) and recedes when anteroposterior pressure applied by the examiner releases the internal impingement (b). Reproduced from XX with permission. | |
In 2002, Crockett et al. highlighted a torsional adaptation of the humerus in young throwing athletes during the acceleration phase of throwing, which results in humeral hyper-retroversion, delaying the onset of mechanical impingement on the dominant side.[17]
It is a positive and protective adaptation. Of the 45 arthroscopic debridement failures, Walch et al. then proposed 20 humeral derotational osteotomies, the results of which were reported by Riand et al. (Figure 13).[18]
Derotational osteotomy
Whereas 80% of the patients were satisfied or very satisfied with reduced cocking pain through release of the impingement, only 55% of them were able to resume their sport at the same level. This is ambitious surgery, requiring great motivation and understanding because a return to sports can be considered only after 6 months, and a return to the same performance level after 12 months. Surgery repetition is often necessary to remove hardware and/or release adhesions. The loss of internal rotation is on average 4 vertebrae (1 to 8), which the patient should be informed of preoperatively.
The best results were reported in cases involving young, ambitious athletes with low humeral retroversion (<10 degrees preoperatively, the goal being to obtain 30 degrees retroversion postoperatively). Poor results were found in cases of hyperlaxity (a factor of poor shoulder stabilization), excessive preoperative retroversion (> 20 degrees) or overcompensation (responsible for anterior impingement between the lesser tubercle and the anterior glenoid), and undercompensation (<10 degrees). The authors reported complications in 30% of cases, including 4 of stiffness, 2 revisions (1 hematoma drainage and 1 nonunion) and 16 requiring hardware removal.[14]
Functional theory
In 1995, Kibler et al. introduced the concept of a kinetic chain encompassing all the body parts that participate in the throwing action, including the whipping movement developed by the shoulder muscles when playing tennis. He proposed that the leg-trunk unit behaves like a force actuator; the arm’s role is to deliver the stored energy and the shoulder acts as a regulator to suitably transmit velocity and energy. A good glenoid-to-humerus alignment allows maximum muscle efficiency, maximum glenoid-to-humerus compression, and frees the shoulder’s rotational movements, which act like a catapult when throwing. Kibler et al. insist that the entire muscle chain must be strengthened to prevent injuries and increase efficiency.[19]
They also recommend conservative treatment, relying on numerous unpublished publications (from the late 1980s till present), dominated mainly by the analysis of baseball pitchers.[20]
In a 2013 article, Kibler et al. further refined their analysis based on their well-known and widely circulated protocol. They review all dysfunctions to be corrected, insist on the value of rehabilitation and recommend caution before considering a surgery because the tears are often adaptive.
Since surgery rarely allows return to sports at the same level, prevention plays an important role. Kibler et al. are very critical when analyzing the results of surgical treatment, which are highly variable, probably due to the very different selection of patients from one author to another, but there is also no precise postoperative follow-up of the tears treated, their localization, concomitant pathologies, and the type of postoperative rehabilitation protocol. Patient motivation is also difficult to gauge. It is therefore important to identify shoulders at risk, typically where one shoulder is lower than the other, with internal or glenohumeral rotation deficits (Figure 14) and scapular dysfunctions or ‘SICK scapula’ ( S: Scapular malposition, I: Inferior medial corner prominence, C: Coracoid pain and malposition, K: Kinesis abnormalities of scapular movements; please, refer Clinical Examination/Inspection section).
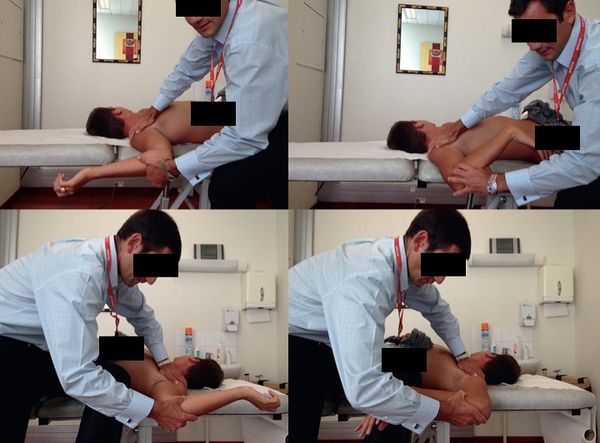
Scapulothoracic dyskinesia is characterized by detachment of the medial scapular rim, observing the comparative posterior scapulothoracic movements, while the patient raises and lowers both upper limbs in the scapular plane. Stiffness of the pectoralis minor can also be identified. Kibler et al. show that glenohumeral internal rotation deficit (GIRD) and SICK (please, refer Clinical Examination/Inspection section) disrupt glenohumeral kinematics. They establish a direct relationship between these dysfunctions and the occurrence of tears, although it is not known how they are causally linked. But they do indicate a strong correlation with increased injury risk, and that preventive rehabilitation reduces these risks.[20]
For example, preventive internal rotation stretching (Figure 15) reduces the risk of injury by 38%.[21]
Sleeper stretch
Regarding motion of the glenohumeral joint, the range in internal and external rotation should remain constant between the dominant and the non-dominant arm, with a shift in the external rotation sector of the dominant arm in overhead throwers (Figure 15).[22]
The rotational 180 degrees rule has not been confirmed (Figure 16), as the mean values of the range of motion is around twice smaller in tennis and handball players.[15][23]
Even if to increase throwing power the athlete moves their total rotational range of motion towards an external hyper-rotation at the expense of internal rotation. In comparative terms, a glenohumeral internal rotation deficit (GIRD) > 20 degrees and a total range of motion asymmetry > 5 degrees represent a shoulder at risk.
The deceleration phase after throwing is the movement most likely to initiate tears. The main role of the external rotators is to brake and dissipate all the energy accumulated during the acceleration phase, which is transmitted by the rotation of the trunk and lower limbs and concentric internal rotators. It is therefore in eccentric contraction that the external rotators will play this part. Repeated eccentric overload stresses result in intramuscular microtears with chronic inflammation, leading to progressive loss of strength and breaking power; hence the imbalance between the external rotators to internal rotators ratio and the occurrence of injuries. Internal rotators work differently because they are stretching during the cocking phase and concentrically contracting during the acceleration phase.[24]
The vast majority of studies shows ratios unfavorable to external rotators on the dominant side, between 0.6 and 0.8. In asymptomatic throwers, the internal rotators are stronger than the external rotators on the dominant side, with an average external rotators to internal rotators ratio of 2:3 (ranging from 60% to 80%). In a population of professional baseball pitchers Byram and co-authors showed that external rotator weakening (with a low external rotators to internal rotators ratio) significantly increases the likelihood of injury. Therefore, it is important to rebalance these ratios by strengthening the external rotators to prevent injuries. In case of pain, Wilk et al. recommend a minimum ratio of 66% to allow recovery.[24][25][26]
Proprioception is more difficult to quantify than range of motion and muscle strength, but some studies have shown that external hyper-rotation, hyperlaxity and repeated trauma to the joint capsule on the thrower’s dominant side are accompanied by worsening spatial perception of the limb, that can explain loss of control injuries.[27][28]
Some authors, such as Kibler et al. or Wilk et al. recommend specific, preventive or curative rehabilitation (pre- or postoperative, using a protocol of stretching, proprioception and muscle strengthening).[26][29]
Theory of the cascade of pathological events or posterosuperior instability and superior labral tear from anterior to posterior (SLAP) lesion pathogenesis.
Starting in 1998, Burkhart, Morgan and Kibler collaborated on a consensual explanation unifying the abovementioned findings. The authors constructed a rational, biomechanical interpretation in the form of a cascade of events involving all the symptoms and tears in thrower’s shoulder. They summarized all the throwing athlete’s dysfunctions and pathologies and conceptualized a theory, which while certainly rational remains very theoretical, because the lack of validation on cadaveric or clinical models (difficult to achieve) makes it unverifiable. Nevertheless, they reject both the micro-instability and biomechanical impingement theories.[22][30]
Suprascapular neuropathy in repetitive overhead athletes
This subsection does not exist. You can ask for it to be created, but consider checking the search results below to see whether the topic is already covered.
Long thoracic nerve injury in repetitive overhead athletes
This subsection does not exist. You can ask for it to be created, but consider checking the search results below to see whether the topic is already covered.
Diagnosis
Anamnesis
A lengthy consultation with the patient is requiredIn to understand the often-multifactorial origin of the problem. The patient’s age, gender, dominant side, and motivation; the type of sport, the performance level and the professional aspect are already vital indicators. Next, is to understand the onset: was it a single trauma (compressive or distractive), repeated microtrauma (cocking and throwing), or progressive (chronic) without trauma. A technopathy should be considered, by asking patients what equipment they use (recent change of racquet, etc.). All previous treatments (conservative and surgical) must be meticulously explained. Merely noting whether patients had rehabilitation is insufficient, because there is a considerable difference between a simple electrotherapy with massages and a complete Kibler protocol.
Clinical examination
The clinical examination must be thorough, especially as a guide to other different diagnoses, such as headaches, instability, acromioclavicular pathology, upper limb neuropathies, vascular disorders of the cervicothoracic junction, and problems of cervical origin and osteopathic disturbances, which do not fit into this nosological framework.
Inspection
The following must be checked: A shoulder that is ‘too low’; Atrophy (supra- or infraspinous fossa) suggesting a neurological diagnosis; Scapulothoracic dyskinesia (SICK scapula; Figure 17). Static scapular malposition in 3 directions in reference to contralateral shoulder (Figure 17): inferior - difference in vertical height (cm); lateral - difference in lateral displacement (cm); abduction - difference in angular degrees of medial scapular margin from plumb midline
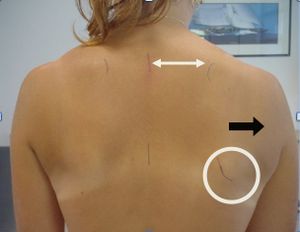
The patient must give an exact description of the sporting movement, directly or with videos, to identify the phase in which pain occurs (cocking, throwing or both).
Palpation
Examination of cervical vertebrae and search for a minor intervertebral osteopathic disorder. Palpation of the acromioclavicular joint, coracoid and bicipital groove.
Evaluation of mobility of other articular joints in the body
The back and legs should be examined, including lumbar mobility, especially the internal rotation of the contralateral hip, and concluded in the single-leg stance. A complete physiotherapy assessment can help to define, for example, muscle weakness.
Non-specific tests
Anterior subacromial impingement tests might appear false-positive. During rotator cuff testing, frequently there is pain and loss of strength in Jobe's maneuver, less frequently in Patte’s maneuver or in resisted external rotation (ER1). Signs of hyperlaxity indicate a bad prognosis. Instability tests can be painful, but usually give no clear apprehension or subluxation. Relocation test is usually positive in posterosuperior impingement (Figure 18).
Relocation test

Articular range of motion tests
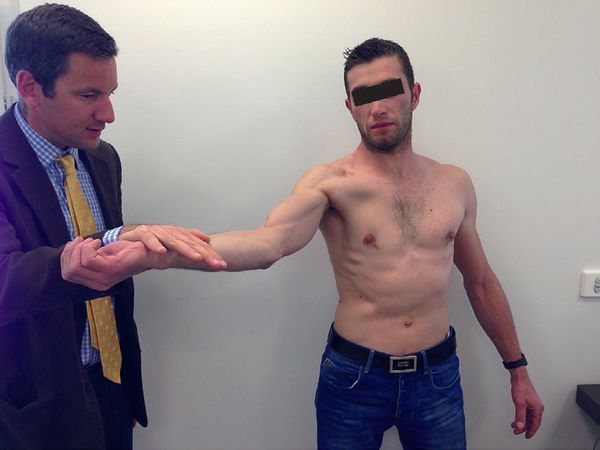
The patient must be examined not only in the standing position, but also supine on a table in order to block scapulothoracic movements, and checked for: All amplitudes (anterior elevation, abduction-internal rotation, ER1, ER2, IR2); Glenohumeral internal rotation deficit (GIRD) > 20 degrees and total range of motion deficit > 5 degrees in the comparative examination.
Specific tests for superior labral tear from anterior to posterior (SLAP) lesions
The literature is particularly rich on this subject, with almost as many different tests as publications. Despite the often-flattering initial reliability of their promoters, it should be noted that few of these tests are used by other practitioners. In their 2009 meta-analysis Meserve et al. retain only 6 valid articles out of 198 initially identified publications (defined by the presence of a descriptive MRI, arthroscopic or arthrotomy reference to the tear, a test used by at least two authors, and the exclusion of cadaveric studies). At the end only the three best tests were retained that could be consequently adopted.[32]
Dynamic Labral Shear test (O’Driscol test)
Shoulder is placed in the extreme abducted and externally rotated position. From this position a valgus stress is applied and a positive response is signified by pain at the shoulder.[33]
Active compression test (better known as O’Brien’s test)
It is an active elevation against resistance, with the patient standing, shoulder flexed at 90 degrees and adducted at 15 degrees, elbow extended (Figure 19). The test is considered positive, if there is pain in pronation but not in supination. This is the most sensitive (47% to 78%), but the least specific (11% to 73%) test. When test is negative, a superior labral tear from anterior to posterior (SLAP) lesion is very unlikely.
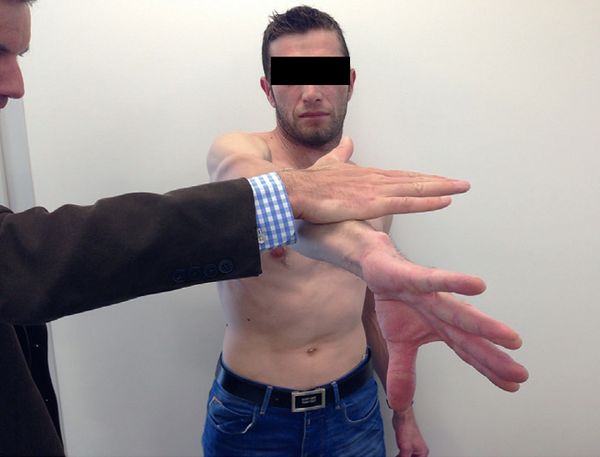
Crank test
The examiner stabilizes the scapula with one hand and keeps the elbow flexed at 90 degrees with the other, applying centripetal force in the humeral axis at 160 degrees abduction, and small medial and lateral rotational movements. Pain indicates a positive test. Sensitivity varies from 13% to 58%, while specificity ranges from 56% to 83% depending on the study. A positive result for this test, in addition to the O'Brien test, reinforces the diagnostic suspicion of superior labral tear.
Speed or Palm-up test
This is a resisted elevation test in the scapular plane in supination at 90 degrees of elevation (Figure 21). Pain indicates a positive test. This is the least sensitive (4% to 48%), but the most specific (67% to 99%) test. A negative result, therefore, indicates the unlikelihood of superior labral tear, but a positive result in all three tests is pathognomonic of a superior labral tear from anterior to posterior (SLAP) lesion.
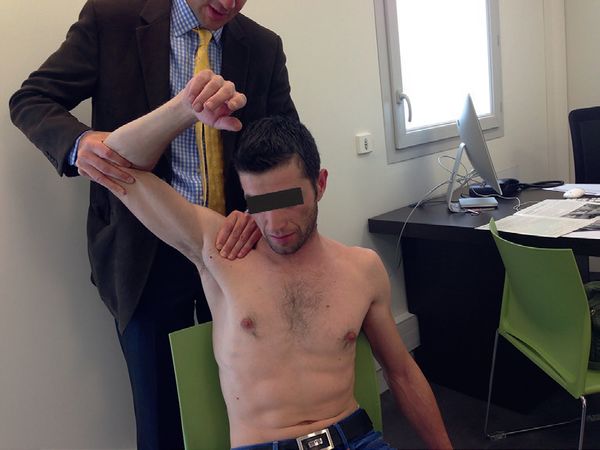
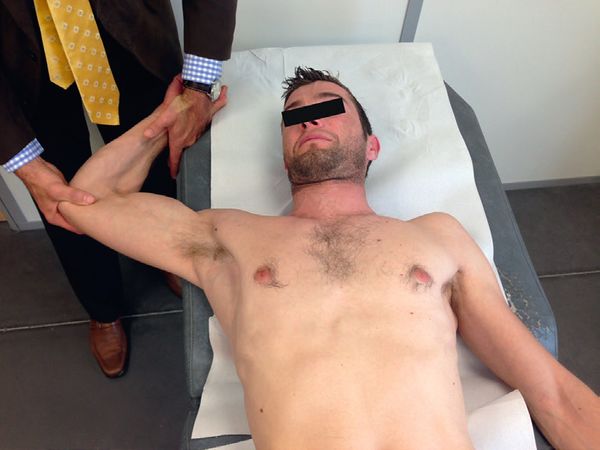
Kim’s test
Kim's test is also worth mentioning (Figure 22), it seems promising, but needs to be validated. The patient is supine with the arm abducted at 120 degrees. The examiner takes the patient's wrist with one hand, while the elbow flexed at 90 degrees is in the other hand. The shoulder is brought into external rotation. Then the patient is asked to flex his elbow against resistance. Deep pain indicates the presence of a superior labral tear from anterior to posterior (SLAP) lesion.[34]
Imaging
There is globally a high incidence of SLAP tears in people over 40 years old as well as a high incidence of incidental lesions in professional baseball pitchers. This should be always taken into account when analysing images.
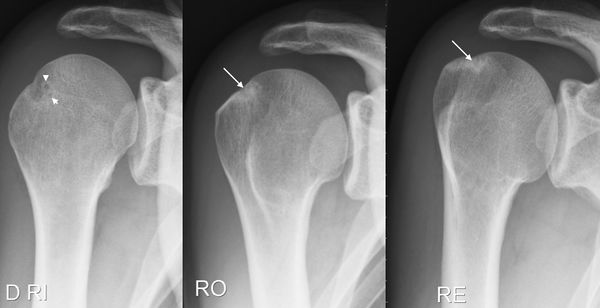
X-ray
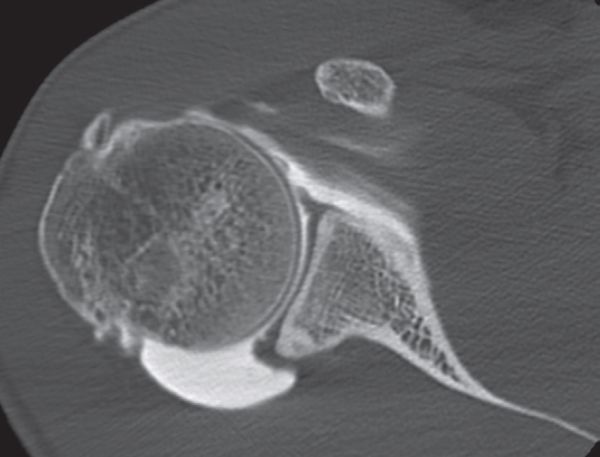
Simple radiographic examination consists of three views: anteroposterior, Lamy and Bernageau. Condensation or bone cysts on the greater tubercle and glenoid rim should be investigated for previous posterosuperior impingements (Figure 23).
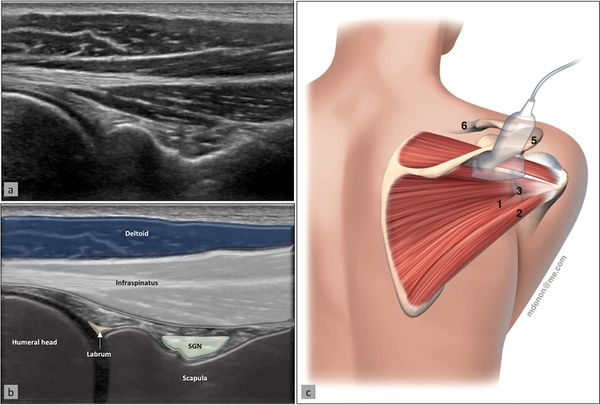
Ultrasonography (US)
Posterior internal impingement occurs often in overhead athletes and involves pinching of the supra- and infraspinatus tendons with the posterosuperior portion of the glenoid labrum, when the shoulder is in abduction/external rotation/hyperextension. Dynamic imaging of this pathological impaction is carried out with the patient’s arm adducted and making external and internal rotation movements (Figure 24).
Computed tomography (CT) and magnetic resonance arthrography (MRA)
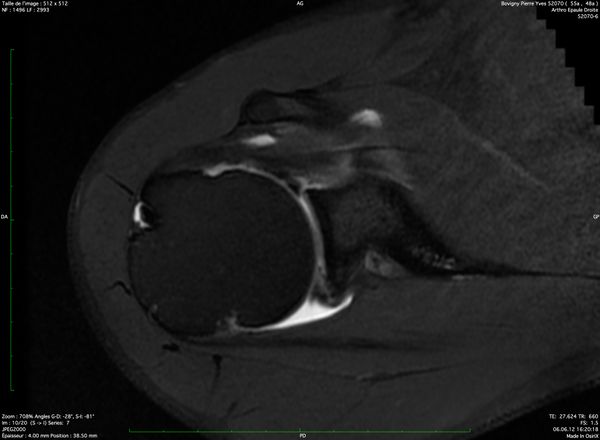
Examinations using intra-articular injection of a contrast medium (CT and MRA) are more reliable than simple MRI to visualize labral lesions and articular rotator cuff lesions (Figures 25-27).
Magnetic resonance arthrography (MRA) finding
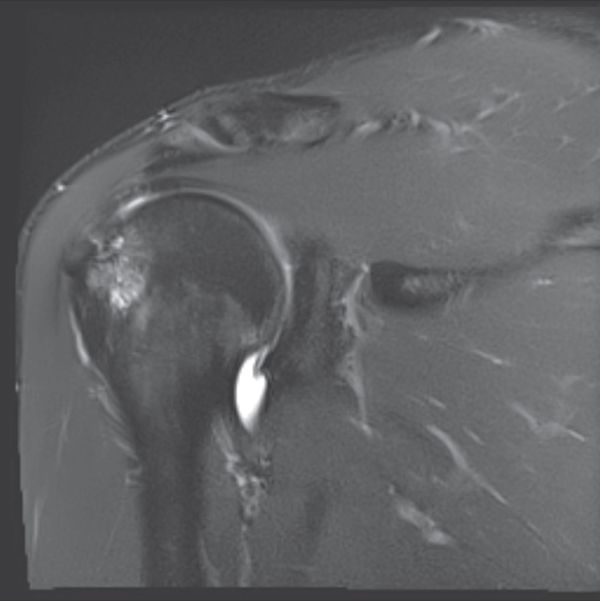
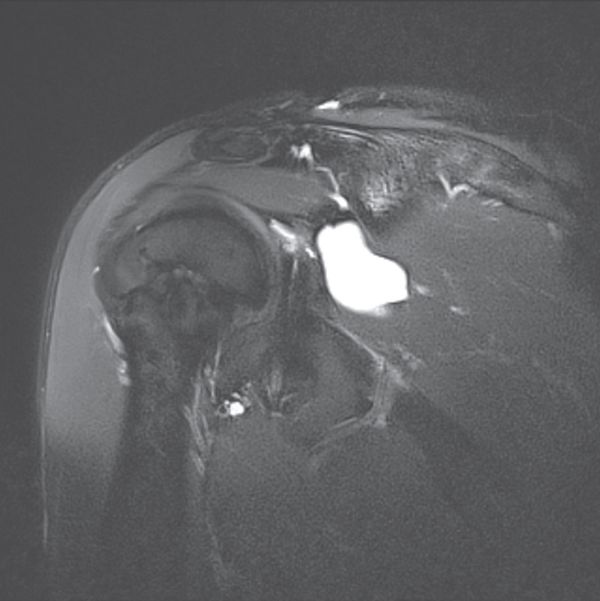
Magnetic resonance arthrography (MRA) is standard, because it can also reveal the possible presence of a paraglenoid cyst (Figure 28) communicating with a labral tear, while allowing analysis of any concomitant tears (rotator cuff, osteochondral), and eliminate other causes of pain (acromioclavicular arthropathy, subacromial bursitis, tears relating to a painful and unstable shoulder).
Reliability depends on both machine and operator efficacy, but Jung et al. report a sensitivity of 85% and a specificity of 86% for superior labral tears.[37]
ABER position further improve sensitivity.[38]
Isokinetic assessment
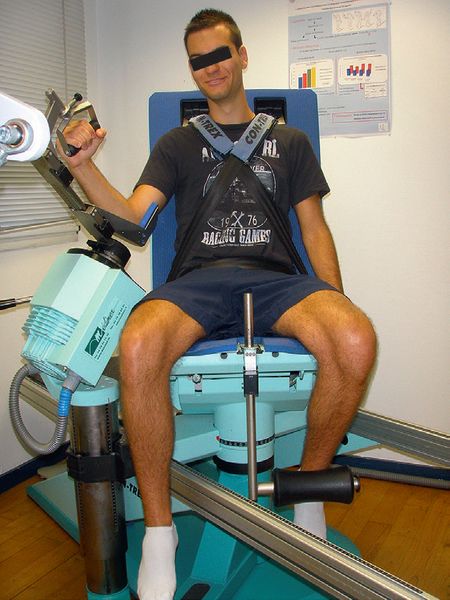
Now isokinetic studies (Figure 29) permit objective quantification of internal and external rotational forces, and especially the definition of ratios for comparative purposes.[39][40]
A mechanical isokinetic assessment, while not perfectly simulating throwing conditions, does ensure a reliable, reproducible method for analyzing ratios and their imbalance, with linear tracking over time (to track progress, etc.). It is of major interest because it must be standardized, just as the articular amplitudes must be perfectly symmetrical before considering surgery or return to sports (with or without surgery).
Arthroscopic assessment
Advanced imaging reduces the usefulness of arthroscopic assessment, which should be reserved for very demanding and motivated patients, to ensure that there are no previously unknown tears. The arm must remain free in order to perform the dynamic cocking maneuver while looking for impingement.
Treatment
Technopathy and sports technique correction
Tennis coaches have begun to modify the service action in such a way as to minimize the damage it causes. This is exemplified by Roddick’s compact service, which replaced the more extended McEnroe service. Walch et al. insist on suppressing hyperabduction (the arm segment must remain in front of the scapular girdle, and no longer move backwards).
Rehabilitation
The fight against stiffness
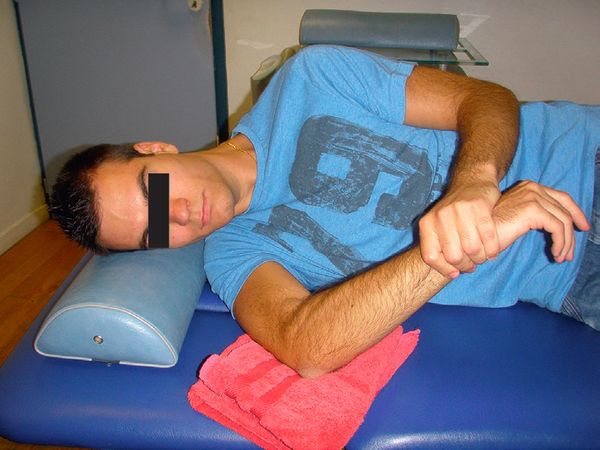
All ranges of movement must be recovered, especially internal rotation at 90 degrees of abduction (IR2), by teaching the patient self-stretching exercises such as ‘sleeper-stretching’ (Figure 30).
Rebalancing the force ratios (external/internal rotators)
Strengthening of the external rotators should be concentric and eccentric using elastics or weights, as described in some protocols depending on the results of the isokinetic analysis (Figure 31).
Proprioception
Proprioception can be worked on with ball exercises (Figure 32).
Surgery
Arthroscopic debridement
Debridement of the labrum (Video 8) and superficial rotator cuff tears renders varying results depending on the author, ranging from 16% for Riand et al. to 85% for Andrews et al.. Labral tears can be left repaired (Figure 33), rotator cuff tears should not be repaired.[5][13]
Arthroscopic arthrolysis
Capsulotomy of the posteroinferior capsule described by Burkhart et al. seems a reasonable option in cases of recalcitrant glenohumeral internal rotation deficit (GIRD), but no isolated capsulotomy study has been conducted to analyze the exact purpose of this surgery. Rehabilitation (sleeper stretching) usually suffices.[21]
Postero-superior glenoidplasty
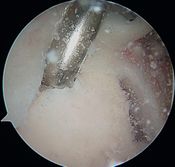
Posterosuperior glenoidplasty described by Levigne et al. (Figure 34 and Video 9) seems to show good results for posterosuperior biomechanical impingement, when posterior osteophytes are clearly visible on the computed tomography (CT) scan.[23][41]
| Figure 34. Glenoidplasty. Arthroscopic view of a right shoulder through an anterolateral portal.
A. Bone spicules on the posterosuperior glenoid rim. B. Post glenoplasty result. Reproduced from XX with permission. | |
Treatment consists of a simple labral resection and liberal milling of the osteophytes and glenoid rim. This minimally invasive and risk-free technique seems very useful, with very good recovery rates at the same sporting level (73%). There are no major complications, notably osteoarthritis or secondary posterior instability at a mean follow-up of 49 months.[23]
Arthroscopic repair of superior labral tear from anterior to posterior (SLAP) lesions
Please, refer also to SLAP chapter.
Sayde et al. reported the results of superior labral tear from anterior to posterior (SLAP) II repairs in a 2012 meta-analysis referencing 14 articles published in English. Inclusion criteria were minimum of 2 years follow-up, assessment of patient satisfaction and/or a return to the same level of sports, superior labral tear from anterior to posterior (SLAP) II tears without associated pathology. Most authors used resorbable implants with knot sutures that seem to give better results. The average follow-up varied from 12 to 44 months. Labral repairs led to good or excellent results in 65% to 95% of cases. On the other hand, surprisingly, analysis of sports recovery at the same performance level was only studied in half the articles, especially since this parameter is always more disappointing than the clinical results with, according to the authors, 44% to 95% of athletes resuming their activity at the same level. Therefore, repairing superior labral tear from anterior to posterior (SLAP) lesions does not seem to solve the problem for throwing athletes.[42]
Gobezie et al. showed a very large variability in the pathogenic role and treatment of superior labral tear from anterior to posterior (SLAP) lesions according to the experts interviewed.
Superior labral tear from anterior to posterior (SLAP) lesions are often adaptations for the thrower (such as increased humeral retroversion) to increase external rotation. Repairing these tears is equivalent to stiffening them and limiting external rotation that allows high-velocity throwing. This explains the poor results of combined repairs (SLAP + rotator cuff) that can end the player's career.
A North American study sounded the alarm during a spate of repairs to superior labral tear from anterior to posterior (SLAP) lesions that in just 20 years tripled from 3.3% (in Snyder's original study) to 9.4%.[43]
Weber et al. even refer to inappropriate surgical indications sometimes involving serious complications with very unexceptional results.[43] The indication could be justified on a real isolated superior labral tear from anterior to posterior (SLAP) II lesion in a patient aged under 30 years having perfectly healthy biceps, or in cases of a painful spinoglenoid cyst. Youm et al. and then Schroder et al. (on a very large series of 42 patients) showed complete regression of the cysts and, therefore, the painful symptoms by repairing only the labral tears without performing any marsupialization of the cyst that can be dangerous due to its attachment to the suprascapular nerve.[44][45]
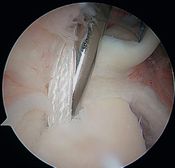
| Figure 35. Arthroscopic SLAP II repair (right shoulder) using the posterior approach (soft point) and knotless anchors. a) Overview of a SLAP II lesion with posterior extension. b) Palpation of a sulcus > 5mm deep. c) Careful bone sharpening. d) Wire threaded by a ‘shuttle relay’ introduced via the Neviaser approach. e) Drilling the anchor-receiving hole. f) Placing the anchor (knotless) to fix the tear backwards. h) Threading a second wire using Bird Peak pliers, introduced by the anterior approach. h) Final assembly. Reproduced from XX with permission. | |||
The beach-chair or supine position, with the arm free and not in traction, allows dynamic tests under arthroscopic control; traction is then optional. The posterior approach (soft point) is lower than usual and slightly lateral, allowing a good view of the posterior labrum. The anterior approach in the rotator interval allows the insertion of a probe to confirm the need for repair. There are three signs required for positive arthroscopic diagnosis of a superior labral tear from anterior to posterior (SLAP) II lesion: a positive peel-back sign during dynamic cocking (the arm is abducted at 90 degrees and externally rotated at 90 degrees), a sublabral sulcus palpation > 5mm deep and a mobile labrobicipital complex. Two secondary instrumental incisions may be performed as required, using a small sleeve (spear guide < 4 mm) that is less traumatic for the rotator cuff and allows threading of anchors. The antero-lateral approach facilitates antero-superior anchoring of the glenoid rim (with an approach angle of 45 degrees) and the posterolateral Wilmington approach (1 cm from the posterolateral acromion angle and 1cm forward) allowing an angle of approach of 45 degrees to the posterosuperior angle of the glenoid.[46]
A specific ancillary procedure using a pointed guide bush maintains the alignment of the instruments and anchor, and quick detection of the incision paths between each surgical step. A motorized burr is used anteriorly to sharpen the superior glenoid rim without removing the bone. One or two small-diameter (3 mm) resorbable anchors with two colored threads are introduced beneath and behind the biceps. Correct alignment of these implants is essential to limit the risk of detachment and to avoid cartilage lesions to the humeral head and glenoid. Wires are threaded through secondary incisions or a modified Neviaser approach, so as to eliminate the peal-back sign.[47]
Biceps tenodesis under arthroscopic control
Please, refer also to biceps tenodesis chapter.
Boileau et al. propose tenodesis of the biceps as an alternative to reparation of superior labral tear from anterior to posterior (SLAP) lesions with satisfactory results, thereby challenging the usefulness of the function preservation of the intra-articular portion of the long head of the biceps, so favored by American authors.[48][49]
The complexity of reproducing the anatomical attachment of the superior labrobicipital complex with its large individual variability and the natural degenerative evolution of the labrum, especially in patients aged over 30 years, favors tenodesis in patients over 35 years of age or with concomitant injuries to the rotator cuff, biceps etc. The reader may refer to the tenodesis chapter for the technical aspect.[50][51][52][53]
Arthroscopic rotator cuff repair
If the aim is a return to sports activity at the same level, the literature reports better results for debridement rather than repair. There is, however, a selection bias. It seems that the indication for repair relates more to the size of the partial-thickness articular tear (> 50% of its insertion or Ellman grades 2 and 3), indicating a serious development of the thrower’s shoulder pain. Therefore, whereas repairing the rotator cuff results in a good functional index allowing return to sports, it may also spell the sudden end of the professional athlete’s career.[54][55]
Derotational osteotomy
This is an invasive procedure reserved only for top level young athletes who are motivated and aware of the risks (Figure 36). In any case, the patient must be informed of all possible complications. The indications remain exceptional.[18]
Conclusion
A thrower’s shoulder consultation is time-consuming and should not result in a surgical indication until all muscle amplitudes and deficits have been rebalanced, and any scapulothoracic dyskinesia corrected. When surgery is indicated, the surgeon should not try to fix everything and should remember the ‘salvage’ nature of the procedure, because even if the published results show improved functional scores, only half of the patients return to the same sporting level, whatever technique is used. The observed tears are often adaptive and only the main cause of pain preventing the patient’s athletic activity should be identified and treated. Surgical escalation on concomitant lesions can lead to stiffness, preventing the patient from a return to previous athletic performance. Severe rotator cuff injury often spells the end of a professional sports career.
Swimmer's Shoulder
From [56], with permission.
Introduction
Swimmers have a significant potential for shoulder injuries due to the unique nature of the different strokes involved in swimming as well as the high volume of repetitions needed during training. Swimmer’s shoulder is a term that can represent numerous shoulder pathologies. These include impingement syndrome, rotator cuff tendinitis, labral injuries, instability secondary to ligamentous laxity or muscle imbalance/dysfunction, neuropathy from nerve entrapment, and anatomic variants. In order for the athlete to return to the sport in an appropriate and timely manner, the clinician must be able to differentiate between these different etiologies.[57]
Etiology
Swimming is a unique activity because it requires primarily the upper body for the propulsive force, with 90% of the driving force provided primarily by the torque generated from the shoulder. To swim at an elite level each swimmer must log between 60,000 and 80,000 meters per week, which is equivalent to 30,000 strokes per arm. Fundamentally, the swim stroke requires the shoulder to move to range-of-motion extremes while tremendous muscular force is exerted upon the shoulder.[58][59][60]
Epidemiology
The incidence of swimmer's shoulder, depending on the study, ranges from 3% to 70%. When defined as shoulder pain that interferes with training or progress in training, the incidence is reported as approximately 35% in elite and senior level swimmers.[61]
Pathophysiology
Swimming strokes can be broken down into pull-through and recovery phases. The latissimus dorsi and the pectoralis major are the primary contributors to propulsive forces of the swim stroke by adduction and internal rotation. The subscapularis and serratus anterior muscles also play an integral role in the freestyle stroke.[61][62][63][64]The freestyle stroke can be divided into six distinct parts/phases:
- Hand entry
- Forward reach
- Pull through
- Middle pull through
- Hand exit
- Middle recovery
It is important for the athlete to have a properly balanced shoulder regarding muscle strength. Improper muscle balancing can cause the onset of shoulder pain. An absolute or sudden increase in training yardage and poor technique can also be associated with the onset of pain. The coaching staff can observe a dropped elbow during the recovery phase of the freestyle stroke as one of the early signs of possible injury.
History and Physical
As is the case with most physical ailments of the body, a thorough physical examination is imperative for diagnosing a swimmer’s shoulder pain. The shoulders should be checked for atrophy and symmetry, the range of motion should be measured. Special attention should be paid to scapular positioning at rest and symmetry in motion to assess for abnormal motion. Strength testing likely will produce pain, and in advanced cases, the shoulder may fail to resist the examiner’s force.
Special testing may provide further insight. The apprehension/relocation test and sulcus signs provide insight into instability. The Hawkins test is a useful and sensitive exam in the diagnosis of subacromial impingement. In patients with positive laxity test results, the examiner also should check other joints for laxity to rule out a generalized condition.[62]
Evaluation
Plain radiographs are obtained initially to rule out any abnormal anatomic variations. Following evaluation by a sports medicine physician, an MRI may be ordered to better identify pathology in the muscles, tendons, ligaments, and cartilage or to exclude other structural causes, such as labral cysts. Although many shoulder diagnoses can be reached based on the physical examination alone, MRI is useful in confirming a diagnosis or when shoulder pain appears to have more than one source. An MRI arthrogram can be considered, when a labral or tendon tear is suspected. Although imaging is an important part of the diagnosis, caution is warranted in interpreting imaging because repetitive motion creates asymptomatic pathology in many athletes.
Treatment / Management
Nonsurgical Management
Eliminating acute inflammation is the priority in shoulder rehabilitation. After a swimmer, first experiences pain, ice, NSAIDs, and rest can prevent progression. If pain continues or worsens, a 7-day to 10-day course of NSAIDs and rest is ideal but often proves difficult, if the injury occurs during the middle or late part of the season. At a minimum, effort should be made to reduce yardage to below the point of pain. For swimmers with impingement, tendinitis, or scapular dyskinesis, a subacromial and/or glenohumeral corticosteroid injection may be beneficial diagnostically and for pain reduction.[65][66]
Stretches that focus on the posterior capsule are important for preventing and reversing impingement. When they are coupled with overstretching of the anterior capsule, swimmers can create imbalances that worsen impingement. The swimmer can stretch the posterior capsule by horizontally adducting the arm and using the contralateral arm to pin it against the body.
Disproportionately increased adduction strength and internal rotation are unavoidable consequences of swimming. Overdevelopment of the pectoralis major and latissimus dorsi muscle groups creates a force that displaces the humeral head anteriorly, leading to joint instability. Additionally, rotator cuff strengthening will lead to muscular balance restoration, which will reduce or eliminate impingement. As muscle endurance and strength improve, sport-mimicking exercises can be attempted, followed by low-yardage workouts at slow speeds, as long as the swimmer is pain-free, and progressing slowly until the swimmer can return to competition.[67][68]
Surgical Management
Surgery is appropriate for structural pathologies. An athlete may elect symptomatic management rather than surgery, so that he or she may continue competing until the pain begins to interfere with daily life. For swimmers with persistent multidirectional instability, a capsular plication or inferior capsular shift procedure should be considered. Athletes should be aware. However, that training volumes may need to be reduced permanently to avoid pain. A subacromial exploration and removal of the hypertrophied, inflamed, and scarred tissue (thereby maintaining the structural integrity of the shoulder) is an option for athletes who obtain only limited relief from physical therapy. For swimmers with a labral tear in whom nonsurgical treatment has failed, the next treatment option is labral debridement or repair.
Enhancing Healthcare Team Outcomes
Swimmer's shoulder is best managed by an interprofessional team that includes the orthopedic nurse. The shoulder provides the greatest range of motion of all joints in the body, but also possesses the greatest inherent instability. As a result of the complexities, combinations, and variations encountered when examining the painful swimmer’s shoulder, a correct diagnosis can be challenging. A range of provocative tests and imaging studies is critical in identifying the pain source and in determining the appropriate treatment. Although some pathology may be managed symptomatically by ice and NSAIDs, athletes with persistent pain should seek evaluation by a sports medicine physician, who may be able to offer more aggressive treatments. Physical therapy can be especially helpful in balancing muscle groups, reducing in-season symptoms, and potentially preventing future injuries.
Most swimmers do have a good outcome with treatment, but recurrence is not uncommon. Hence, the efforts of a strong interprofessional team for ongoing management will yield the best patient results.[69]
References
- ↑ Reproduced from Barth J, Graveleau N, Jouve F, Barthélémy R. Diagnostic et traitement de l'épaule du lanceur. In: Société Française D'Arthroscopie PJ, Hulet C., ed. L’arthroscopie. Paris: Elsevier Masson; 2015, with permission.
- ↑ Neer CS, 2nd. Anterior acromioplasty for the chronic impingement syndrome in the shoulder: a preliminary report. J Bone Joint Surg Am 1972;54:41-50.
- ↑ Tibone JE, Jobe FW, Kerlan RK, et al. Shoulder impingement syndrome in athletes treated by an anterior acromioplasty. Clin Orthop Relat Res 1985:134-40.
- ↑ Jobe FW, Giangarra CE, Kvitne RS, Glousman RE. Anterior capsulolabral reconstruction of the shoulder in athletes in overhand sports. Am J Sports Med 1991;19:428-34.
- ↑ 5.0 5.1 5.2 Andrews JR, Carson WG, Jr., McLeod WD. Glenoid labrum tears related to the long head of the biceps. Am J Sports Med 1985;13:337-41.
- ↑ 6.0 6.1 Burkhart SS, Morgan CD. The peel-back mechanism: its role in producing and extending posterior type II SLAP lesions and its effect on SLAP repair rehabilitation. Arthroscopy 1998;14:637-40.
- ↑ 7.0 7.1 Snyder SJ, Karzel RP, Del Pizzo W, Ferkel RD, Friedman MJ. SLAP lesions of the shoulder. Arthroscopy 1990;6:274-9.
- ↑ Bey MJ, Elders GJ, Huston LJ, Kuhn JE, Blasier RB, Soslowsky LJ. The mechanism of creation of superior labrum, anterior, and posterior lesions in a dynamic biomechanical model of the shoulder: the role of inferior subluxation. J Shoulder Elbow Surg 1998;7:397-401.
- ↑ Clavert P, Bonnomet F, Kempf JF, Boutemy P, Braun M, Kahn JL. Contribution to the study of the pathogenesis of type II superior labrum anterior-posterior lesions: a cadaveric model of a fall on the outstretched hand. J Shoulder Elbow Surg 2004;13:45-50.
- ↑ Jobe CM. Posterior superior glenoid impingement: expanded spectrum. Arthroscopy 1995;11:530-6.
- ↑ Walch G, Boileau P, Noel E, Donell ST. Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-45.
- ↑ Sonnery-Cottet B, Edwards TB, Noel E, Walch G. Results of arthroscopic treatment of posterosuperior glenoid impingement in tennis players. Am J Sports Med 2002;30:227-32.
- ↑ 13.0 13.1 Riand N, Boulahia A, Walch G. [Posterosuperior impingement of the shoulder in the athlete: results of arthroscopic debridement in 75 patients]. Rev Chir Orthop Reparatrice Appar Mot 2002;88:19-27.
- ↑ 14.0 14.1 Edwards B, Walch G. Posterosuperior glenoid impingement : Is microinstability really the problem ? Operative Techniques in Sports Medicine 2002;10:40-6.
- ↑ 15.0 15.1 Lädermann A, Chague S, Kolo FC, Charbonnier C. Kinematics of the shoulder joint in tennis players. Journal of science and medicine in sport 2016;19:56-63.
- ↑ Davidson PA, Elattrache NS, Jobe CM, Jobe FW. Rotator cuff and posterior-superior glenoid labrum injury associated with increased glenohumeral motion: a new site of impingement. J Shoulder Elbow Surg 1995;4:384-90.
- ↑ Crockett HC, Gross LB, Wilk KE, et al. Osseous adaptation and range of motion at the glenohumeral joint in professional baseball pitchers. Am J Sports Med 2002;30:20-6.
- ↑ 18.0 18.1 Riand N, Levigne C, Renaud E, Walch G. Results of derotational humeral osteotomy in posterosuperior glenoid impingement. Am J Sports Med 1998;26:453-9.
- ↑ Kibler WB. Biomechanical analysis of the shoulder during tennis activities. Clinics in sports medicine 1995;14:79-85.
- ↑ 20.0 20.1 Kibler WB, Kuhn JE, Wilk K, et al. The disabled throwing shoulder: spectrum of pathology-10-year update. Arthroscopy 2013;29:141-61 e26.
- ↑ 21.0 21.1 Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology. Part II: evaluation and treatment of SLAP lesions in throwers. Arthroscopy 2003;19:531-9.
- ↑ 22.0 22.1 Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part I: pathoanatomy and biomechanics. Arthroscopy 2003;19:404-20.
- ↑ 23.0 23.1 23.2 Levigne C, Garret J, Grosclaude S, Borel F, Walch G. Surgical technique arthroscopic posterior glenoidplasty for posterosuperior glenoid impingement in throwing athletes. Clin Orthop Relat Res 2012;470:1571-8.
- ↑ 24.0 24.1 Byram IR, Bushnell BD, Dugger K, Charron K, Harrell FE, Jr., Noonan TJ. Preseason shoulder strength measurements in professional baseball pitchers: identifying players at risk for injury. Am J Sports Med 2010;38:1375-82.
- ↑ Mikesky AE, Edwards JE, Wigglesworth JK, Kunkel S. Eccentric and concentric strength of the shoulder and arm musculature in collegiate baseball pitchers. Am J Sports Med 1995;23:638-42.
- ↑ 26.0 26.1 Wilk KE, Andrews JR, Arrigo CA, Keirns MA, Erber DJ. The strength characteristics of internal and external rotator muscles in professional baseball pitchers. Am J Sports Med 1993;21:61-6.
- ↑ Allegrucci M, Whitney SL, Lephart SM, Irrgang JJ, Fu FH. Shoulder kinesthesia in healthy unilateral athletes participating in upper extremity sports. The Journal of orthopaedic and sports physical therapy 1995;21:220-6.
- ↑ Blasier RB, Carpenter JE, Huston LJ. Shoulder proprioception. Effect of joint laxity, joint position, and direction of motion. Orthop Rev 1994;23:45-50.
- ↑ Kibler WB, Kuhn JE, Wilk K, et al. The disabled throwing shoulder: spectrum of pathology-10-year update. Arthroscopy 2013;29:141-61 e26.
- ↑ Burkhart SS, Morgan CD, Kibler WB. Shoulder injuries in overhead athletes. The "dead arm" revisited. Clinics in sports medicine 2000;19:125-58.
- ↑ Jobe F, Tibone J, Jobe C, Kvitne R. The shoulder in sports. In: Rockwood CA MF, eds. , ed. The shoulder. Philadelphia: WB Saunders; 1990:961-90.
- ↑ Meserve BB, Cleland JA, Boucher TR. A meta-analysis examining clinical test utility for assessing superior labral anterior posterior lesions. Am J Sports Med 2009;37:2252-8.
- ↑ Cook C, Beaty S, Kissenberth MJ, Siffri P, Pill SG, Hawkins RJ. Diagnostic accuracy of five orthopedic clinical tests for diagnosis of superior labrum anterior posterior (SLAP) lesions. J Shoulder Elbow Surg 2012;21:13-22.
- ↑ Kim SH, Ha KI, Ahn JH, Kim SH, Choi HJ. Biceps load test II: A clinical test for SLAP lesions of the shoulder. Arthroscopy 2001;17:160-4.
- ↑ Pesquer L, Poussange N, Moreau-Durieux M-H, et al. Le conflit postéro-supérieur de l’épaule. Journal de Radiologie Diagnostique et Interventionnelle 2017;98:296-302
- ↑ Plomb-Holmes C, Clavert P, Kolo F, Tay E, Ladermann A, French Arthroscopic S. An orthopaedic surgeon's guide to ultrasound imaging of the healthy, pathological and postoperative shoulder. Orthop Traumatol Surg Res 2018;104:S219-S32
- ↑ Jung JY, Yoon YC, Choi SH, Kwon JW, Yoo J, Choe BK. Three-dimensional isotropic shoulder MR arthrography: comparison with two-dimensional MR arthrography for the diagnosis of labral lesions at 3.0 T. Radiology 2009;250:498-505.
- ↑ Choi JY, Kim SH, Yoo HJ, et al. Superior labral anterior-to-posterior lesions: comparison of external rotation and active supination CT arthrography with neutral CT arthrography. Radiology 2012;263:199-205.
- ↑ Codine P, Bernard PL, Pocholle M, Herisson C. [Isokinetic strength measurement and training of the shoulder: methodology and results]. Annales de readaptation et de medecine physique : revue scientifique de la Societe francaise de reeducation fonctionnelle de readaptation et de medecine physique 2005;48:80-92.
- ↑ Gozlan G, Bensoussan L, Coudreuse JM, et al. [Isokinetic dynamometer measurement of shoulder rotational strength in healthy elite athletes (swimming, volley-ball, tennis): comparison between dominant and nondominant shoulder]. Annales de readaptation et de medecine physique : revue scientifique de la Societe francaise de reeducation fonctionnelle de readaptation et de medecine physique 2006;49:8-15.
- ↑ Lévigne C, Garret J, Borel F, Walch G. Glénoplastie postérieure sous arthroscopie pour conflit glénoïdien postérosupérieur. Rev Chir Orthop Reparatrice Appar Mot 2007;93:37.
- ↑ Sayde WM, Cohen SB, Ciccotti MG, Dodson CC. Return to play after Type II superior labral anterior-posterior lesion repairs in athletes: a systematic review. Clin Orthop Relat Res 2012;470:1595-600.
- ↑ 43.0 43.1 Weber SC, Martin DF, Seiler JG, 3rd, Harrast JJ. Superior labrum anterior and posterior lesions of the shoulder: incidence rates, complications, and outcomes as reported by American Board of Orthopedic Surgery. Part II candidates. Am J Sports Med 2012;40:1538-43.
- ↑ Youm T, Matthews PV, El Attrache NS. Treatment of patients with spinoglenoid cysts associated with superior labral tears without cyst aspiration, debridement, or excision. Arthroscopy 2006;22:548-52.
- ↑ Schroder CP, Skare O, Stiris M, Gjengedal E, Uppheim G, Brox JI. Treatment of labral tears with associated spinoglenoid cysts without cyst decompression. J Bone Joint Surg Am 2008;90:523-30.
- ↑ Lo IK, Lind CC, Burkhart SS. Glenohumeral arthroscopy portals established using an outside-in technique: neurovascular anatomy at risk. Arthroscopy 2004;20:596-602.
- ↑ Nord KD, Masterson JP, Mauck BM. Superior labrum anterior posterior (SLAP) repair using the Neviaser portal. Arthroscopy 2004;20 Suppl 2:129-33.
- ↑ Boileau P, Parratte S, Chuinard C, Roussanne Y, Shia D, Bicknell R. Arthroscopic treatment of isolated type II SLAP lesions: biceps tenodesis as an alternative to reinsertion. Am J Sports Med. 2009 May;37(5):929-36
- ↑ Rojas IL, Provencher MT, Bhatia S, et al. Biceps activity during windmill softball pitching: injury implications and comparison with overhand throwing. Am J Sports Med 2009;37:558-65.
- ↑ Pfahler M, Haraida S, Schulz C, et al. Age-related changes of the glenoid labrum in normal shoulders. J Shoulder Elbow Surg 2003;12:40-52.
- ↑ De Maeseneer M, Van Roy F, Lenchik L, et al. CT and MR arthrography of the normal and pathologic anterosuperior labrum and labral-bicipital complex. Radiographics : a review publication of the Radiological Society of North America, Inc 2000;20 Spec No:S67-81.
- ↑ Vangsness CT, Jr., Jorgenson SS, Watson T, Johnson DL. The origin of the long head of the biceps from the scapula and glenoid labrum. An anatomical study of 100 shoulders. J Bone Joint Surg Br 1994;76:951-4.
- ↑ Denard PJ, Lädermann A, Parsley BK, Burkhart SS. Arthroscopic biceps tenodesis compared with repair of isolated type II SLAP lesions in patients older than 35 years. Orthopedics. 2014 Mar;37(3):e292-7
- ↑ Neri BR, ElAttrache NS, Owsley KC, Mohr K, Yocum LA. Outcome of type II superior labral anterior posterior repairs in elite overhead athletes: Effect of concomitant partial-thickness rotator cuff tears. Am J Sports Med 2011;39:114-20.
- ↑ Sonnery-Cottet B, Edwards TB, Noel E, Walch G. Rotator cuff tears in middle-aged tennis players: results of surgical treatment. Am J Sports Med 2002;30:558-64.
- ↑ Davis DD, Nickerson M, Varacallo M. Swimmer's Shoulder. [Updated 2020 Jun 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-.
- ↑ Varacallo M, El Bitar Y, Mair SD. Rotator Cuff Tendonitis. StatPearls Publishing; Treasure Island (FL): Apr 23, 2020
- ↑ Demarie S, Chirico E, Gianfelici A, Vannozzi G. Anaerobic capacity assessment in elite swimmers through inertial sensors. Physiol Meas. 2019 Jul 03;40(6):064003
- ↑ Lee M, Szuttor K, Holm C. A computational model for bacterial run-and-tumble motion. J Chem Phys. 2019 May 07;150(17):174111
- ↑ Yuan ZM, Li M, Ji CY, Li L, Jia L, Incecik A. Steady hydrodynamic interaction between human swimmers. J R Soc Interface. 2019 Jan 31;16(150):20180768
- ↑ 61.0 61.1 Matzkin E, Suslavich K, Wes D. Swimmer's Shoulder: Painful Shoulder in the Competitive Swimmer. J Am Acad Orthop Surg. 2016 Aug;24(8):527-36
- ↑ 62.0 62.1 De Martino I, Rodeo SA. The Swimmer's Shoulder: Multi-directional Instability. Curr Rev Musculoskelet Med. 2018 Jun;11(2):167-171
- ↑ Tessaro M, Granzotto G, Poser A, Plebani G, Rossi A. SHOULDER PAIN IN COMPETITIVE TEENAGE SWIMMERS AND IT'S PREVENTION: A RETROSPECTIVE EPIDEMIOLOGICAL CROSS SECTIONAL STUDY OF PREVALENCE. Int J Sports Phys Ther. 2017 Oct;12(5):798-811
- ↑ Hibberd EE, Laudner KG, Kucera KL, Berkoff DJ, Yu B, Myers JB. Effect of Swim Training on the Physical Characteristics of Competitive Adolescent Swimmers. Am J Sports Med. 2016 Nov;44(11):2813-2819
- ↑ Kancherla VK, Heckman DS, Carolan GF. Luxatio erecta humeri in the swimmer's shoulder: A combination of ligamentous laxity and motion dyskinesis. J Emerg Trauma Shock. 2016 Jan-Mar;9(1):39-40
- ↑ Hibberd EE, Laudner K, Berkoff DJ, Kucera KL, Yu B, Myers JB. Comparison of Upper Extremity Physical Characteristics Between Adolescent Competitive Swimmers and Nonoverhead Athletes. J Athl Train. 2016 Jan;51(1):65-9
- ↑ de Almeida MO, Hespanhol LC, Lopes AD. PREVALENCE OF MUSCULOSKELETAL PAIN AMONG SWIMMERS IN AN ELITE NATIONAL TOURNAMENT. Int J Sports Phys Ther. 2015 Dec;10(7):1026-34
- ↑ Nichols AW. Medical Care of the Aquatics Athlete. Curr Sports Med Rep. 2015 Sep-Oct;14(5):389-96
- ↑ Tovin BJ. Prevention and Treatment of Swimmer's Shoulder. N Am J Sports Phys Ther. 2006 Nov;1(4):166-75