Shoulder:The Biceps Tendon/Superior Labral Tear from Anterior to Posterior (SLAP) Lesion
Contents
- 1 Bullet Points
- 2 Key Words
- 3 Anatomy
- 4 Treatment
- 5 References
Bullet Points
- Since their initial description in the late 1980’s the etiology, diagnosis and treatment of superior labral tears have been controversial.
- The large number of normal anatomic variants of the superior labrum and the surrounding structures make the interpretation of SLAP challenging on imaging and at arthroscopy.
- The incidence of SLAP lesions increased in time, possibly due to the difficulty in distinguishing a normal pattern from the pathological one.
- A lot of movements can produce a SLAP lesion (compressive, torsional, tensile, shear forces), but the exact mechanism or combination of mechanism remains controversial.
- There is no physical test or sign sufficiently specific for SLAP lesions.
- Magnetic Resonance Arthrogram (MRA) is recognized as the gold standard for SLAP diagnosis.
- Care must be taken to ensure that inappropriate surgical intervention is avoided, particularly in cases where a SLAP lesion is identified “en passant”.
- Different surgical techniques are described. Biceps tenodesis or tenotomy are preferable to biceps repair for isolated type II SLAP lesions in non-overhead athletes older than 35 years.
- Most spinoglenoid cysts resolve after the labral fixation without cyst decompression. Decompression is only recommended in case of suprascapular nerve impairment.
Key Words
Superior Labral Tear from Anterior to Posterior Lesion; SLAP; Long head of the biceps; Variants; Over-head athletes; Throwers; Dead arm syndrome; Spinoglenoid cysts; Suprascapular nerve; Glenohumeral internal rotation deficit; GIRD; Arthroscopic repair; Tenodesis; Tenotomy; Stiffness.
Anatomy
The precise insertion of the tendon of the long head of the biceps muscle can change: it is usually positioned as an extension of the superior glenoid labrum, but it can also be located at the supraglenoid tubercle. Regardless the exact insertion, there is a strong connection between the tendon and the labrum.[1]
Furthermore, Huber and Putz demonstrated that some fibers of the superior glenohumeral ligament are connected with the long head biceps tendon.[2]
The superior portion of the labrum is more mobile compared to the rest of the labrum, and it is more loosely attached. There are some normal variants of the superior and anterosuperior labrum: the sublabral sulcus, the sublabral hole, the Buford complex (absence of the anterior superior labrum in conjunction with a thickened cord-like middle glenohumeral ligament) and other less common variants (Figure 1). It is important not to confuse them with SLAP lesions.[3]
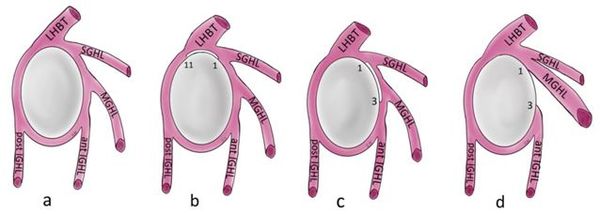
Definition
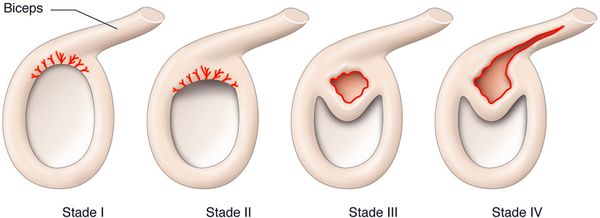
Superior Labrum from Anterior to Posterior (SLAP) lesion is an injury of the superior and anterosuperior portion of the labrum. It’s important to underline that not all SLAP lesions involve long head biceps tendon. Snyder, originally, classified this pathology in 4 groups (Figure 2)[5]
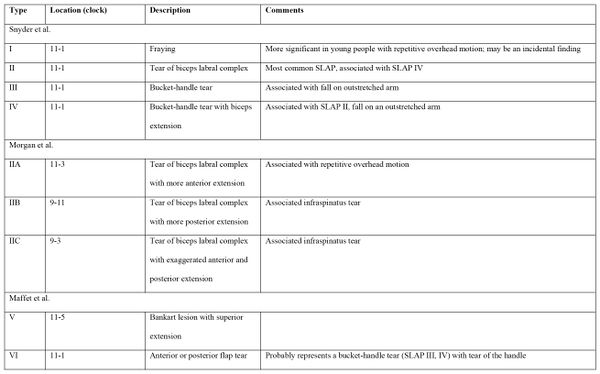
Later some authors divided SLAP II lesions in 3 subtypes: IIA, IIB, IIC.[6]
Further classifications divided SLAP lesions in 10 types.
- V: Bankart lesion (anterior inferior glenolabral injury) with superior extension to include the superior labrum and biceps tendon.
- VI: Flap lesion, anterior or posterior, with separation of the biceps tendon superiorly.
- VII: Superior labrum and biceps tendon separation, involving MGHL.
- VIII: Superior labral tear with posterior extension, similar to IIB type but more extensive.
- IX: Superior tear extended anteriorly and posteriorly, which results in a complete or almost complete detachment of the labrum.
- X: Tear of the labrum with extension into the rotator cuff interval.
Schematic Classification of SLAP lesions
Epidemiology
The real incidence of SLAP lesion is not so clear, but seems to increase over time: originally Snyder reported the incidence lower than 4% (27 SLAP lesions in over 700 shoulder arthroscopies), while Kim and co-authors found out 26% incidence (XX SLAP lesions in 544 shoulders).[5][7]
Between 2002 and 2010, in New York State, the incidence of SLAP repairs increased by a factor of 5.5.[8]
A similar increase was described in the US Active Duty Department of Defense population, where about 6000 operations for SLAP were performed between 2004 and 2008, making it the fourth most common shoulder surgery in that population.[9]
Some authors studied demographic trends of SLAP repair in the United States. They analyzed 25,574 SLAP repairs: 75% were men, and the highest incidence was in the third and fifth decades of life.[10]
The difficulty in distinguishing a normal pattern from a pathological one can explain this trend. In addition, physical examination does not achieve good results, because there is no single test with simultaneous sensitivity and specificity.[11]
Pathogenesis
In older patients SLAP lesions originate from a degenerative process, while in younger patients tear-mechanism is traumatic or micro-traumatic. The most common mechanism is a repeated movement “over-head” or throw-sports. Sports activity is the most frequent cause of repairable SLAP lesions, in particular type II SLAP lesions are most commonly observed in overhead athletes. During throwing over-head movements athletes do a horizontal extension and over rotation. It is interesting to note that in the thrower’s shoulder some adaptive changes has developed over time. Most notably, it is an increase in external rotation and decrease in internal rotation at 90° of abduction. This pattern of motion has been termed “GIRD” (Glenohumeral Internal Rotation Deficit) and has been noted in multiple observational studies of professional baseball players. A lot of movements can produce a SLAP lesion (compressive, torsional, tensile, shear forces), but the exact mechanism or combination of mechanism remains controversial.[5][9]
Associated lesions
Associated lesions of the shoulder, such as lesions of the glenohumeral ligaments, rotator interval, rotator cuff, joint capsule or articular cartilage, could mislead an orthopedic surgeon or a radiologist. It is important to know the existence of some concomitant injuries in order to make a right diagnosis and to better plan the surgical procedure.
Rotator cuff associated lesions include undersurface tears of the supraspinatus and infraspinatus tendons, which are often caused by posterosuperior and anterosuperior internal impingement.
In some cases, Type II SLAP lesions may be associated with the formation of a paralabral cyst. Paralabral cysts associated with Type II SLAP lesions are usually formed in the posterior superior quadrant of the labrum and therefore forms the classical spinoglenoid cyst.
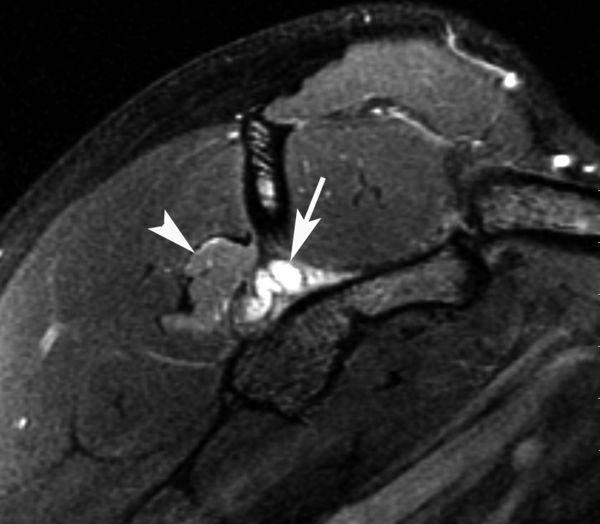
When large, spinoglenoid cysts may encroach upon the suprascapular nerve and result in neuropathy (Figure 3). Unlike suprascapular neuropathy due to compression at the suprascapular notch, suprascapular neuropathy from a spinoglenoid cyst usually results in isolated infraspinatus atrophy and weakness and spares the supraspinatus.
Selective compression of infraspinatus branch of suprascapular nerve.
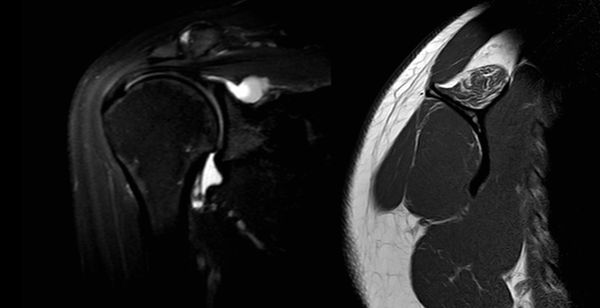
However, a selective compression of the supraspinatus branch is possible (Figure 4).
Selective compression of supraspinatus branch of suprascapular nerve.
Although spontaneous decompression of spinoglenoid cysts may occur, when suprascapular neuropathy is present, decompression of the spinoglenoid cyst is indicated with repair of the superior labral tear.
However, it is important to consider that not all paralabral cyst are associated with SLAP lesions. Many paralabral cysts are the result of degenerative tears of the labrum and osteoarthritis and do not cause suprascapular neuropathy. These cysts usually present more inferior along the glenoid, are smaller and are associated with chondromalacial changes of the glenoid.
Diagnosis
There is no physical test or sign sufficiently specific for SLAP lesions; furthermore, physical findings can be confusing because of the associated lesions. It is difficult to make an accurate clinical diagnosis, so imaging plays an important role in the diagnostic process.
History
The classic patient is a young overhead athlete (age < 30 years) with minimal daily symptoms, but with disability while performing their overhead athletics, the dead arm syndrome. These patients will commonly have confirmatory physical exam findings (O’Brien’s sign, relocation sign for pain) and classic arthroscopic findings of SLAP lesions (see below). In addition, the absence of other pathology (i.e. full thickness tears of the rotator cuff, chondromalacia changes, impingement, etc) is further indicative that the SLAP lesion causes the patient’s symptoms.
In patients over the age of 40 years with an atraumatic onset of symptoms, generalized pain, which is worsened with overhead activities (not necessarily athletics), and other concomitant modifiers (worker’s compensation board, litigation) or conditions (i.e. full thickness tear of the rotator cuff), the diagnosis of a SLAP lesion should be guarded. While an anatomic SLAP lesion may exist on arthroscopic evaluation, many of these patients will have equivocal physical examination findings and the tear of the superior labrum may not be the cause of the symptoms and other concomitant diagnoses should be considered (e.g. rotator cuff tear). In these patients SLAP repair is usually not indicated and one may choose to debride the lesion or perform a biceps tenodesis, if biceps tendinopathy is suspected preoperatively.
Sometimes patients report sensations of clicking, snapping, popping of the shoulder. In some cases long head biceps tendon ruptures can occur and this can reduce the pain.
Clinical evaluation
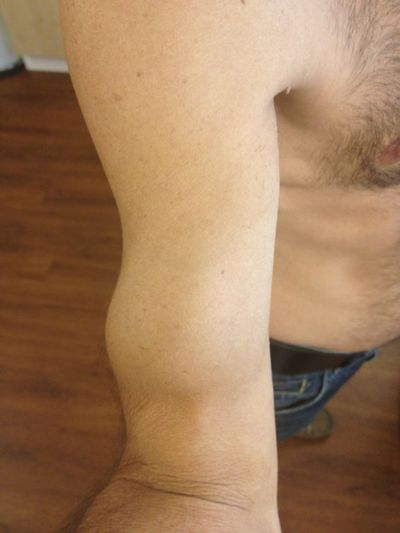
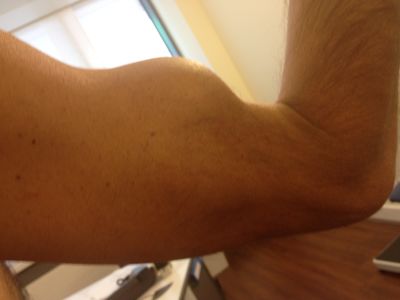
Inspection: it is fundamental to identify deformity or muscular atrophy. Long head biceps tendon rupture causes “Popeye-sign”, which is evident just examining the patient.
Popeye-sign
| Figure 5. Anterior (A) and lateral (B) views of a right arm presenting a Popeye-sign. Reproduced from XX with permission. | |
Palpation
Palpation of the biceps is neither specific nor sensible, but universally painful.
Range of Motion
The patient must be examined not only in the standing position, but also supine on a table to block scapulothoracic movements, and checked for all amplitudes: anterior elevation, abduction, internal rotation and external rotation elbow at the side and at 90 degrees of abduction. Glenohumeral internal rotation deficit (GIRD) > 20 degrees and total range of motion deficit > 5 degrees in the comparative examination.
Tests for superior labral tear from anterior to posterior (SLAP) lesions
The literature is particularly rich on this subject, with almost as many different tests as publications. Despite the often-flattering initial reliability of their promoters, it should be noted that few of these tests are used by other practitioners. Meserve et al. in a meta-analysis retained only 6 valid articles out of 198 initially identified publications (defined by the presence of a descriptive MRI, arthroscopic or arthrotomy reference to the tear, a test used by at least two authors, and the exclusion of cadaveric studies). In the end only the three best tests were retained, which could be consequently adopted.[12]
Dynamic Labral Shear Test (O’Driscol Test)
Shoulder is placed in the extreme abducted and externally rotated position. From this position a valgus stress is applied and a positive response is signified by pain at the shoulder.
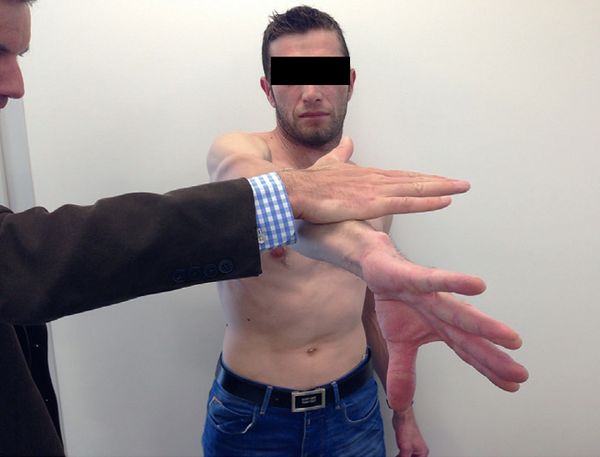
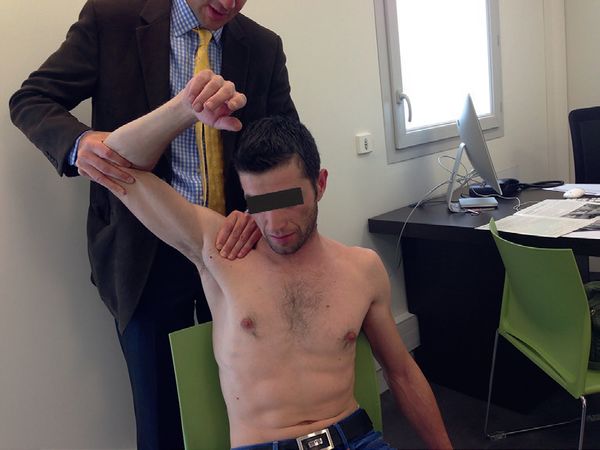
Active Compression Test (O’Brien’s Test):
It is an active elevation against resistance, with the patient standing, shoulder flexed at 90 degrees and adducted at 15 degrees, elbow extended (Figure 6). The test is considered positive, if there is pain in pronation but not in supination. This is the most sensitive (47% to 78%), but the least specific (11% to 73%) test. When test is negative, a superior labral tear from anterior to posterior (SLAP) lesion is very unlikely.
Crank Test
The examiner stabilizes the scapula with one hand and keeps the elbow flexed at 90 degrees with the other, applying centripetal force in the humeral axis at 160 degrees abduction, applying small medial and lateral rotational movements. Pain indicates a positive test. Sensitivity varies from 13% to 58%, while specificity ranges from 56% to 83% depending on the study. A positive result for this test, in addition to the O'Brien test, reinforces the diagnostic suspicion of superior labral tear.
Crank Test
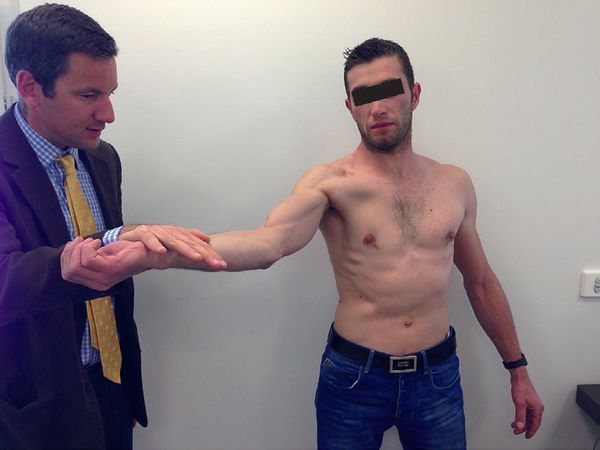
Speed or Palm-up Test
This is a resisted elevation test in the scapular plane in supination at 90 degrees of elevation (Figure 8). Pain indicates a positive test. This is the least sensitive (4% to 48%) but also the most specific (67% to 99%) test. A negative result, therefore, indicates the unlikelihood of superior labral tear, but a positive result in all three tests is pathognomonic of a superior labral tear from anterior to posterior (SLAP) lesion.
Speed or Palm-up Test
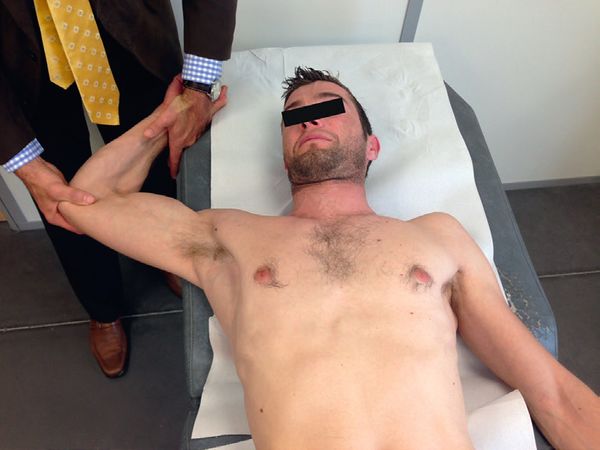
Kim’s Test
The patient is supine with the arm abducted at 120 degrees. The examiner takes the patient's wrist with one hand, while the elbow flexed at 90 degrees is in the other hand. The shoulder is brought into external rotation. The patient is then asked to flex his elbow against resistance. Deep pain indicates the presence of a superior labral tear from anterior to posterior (SLAP) lesion.
Kim Test
Imaging
X-Rays
A shoulder X-ray with standard projection must be always performed, because it could show important aspects of the anatomy and could help with a differential diagnosis. Calcifications, bone deformation or in some cases signs of arthritis can be found. The Fisk projection can show details of the bicipital groove.
Ultrasound (US)
There is no evidence of its utility with SLAP lesions.
Magnetic Resonance Imaging (MRI)
The diagnostic performance of magnetic resonance arthrogram (MRA) is superior to magnetic resonance imaging (MRI) by both direct and indirect comparisons for the detection of SLAP lesions. MRI should not be used for detection of SLAP lesions.[13]
Magnetic Resonance Arthrogram (MRA)
MRA is recognised as the gold standard for SLAP diagnosis. Multiple studies showed high sensitivities and specificities in SLAP lesion diagnosis: sensitivity ranges from 82% to 100%, specificity is between 71% and 98%, accuracy varies between 83% and 94% [29][16]. Intra-articular contrast has reported to be useful to exclude anatomic variants.[13]
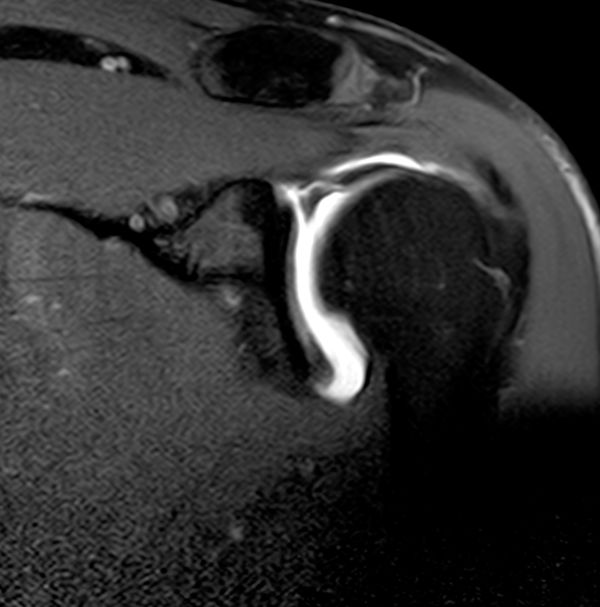
Images in the axial and coronal oblique planes are most useful for the SLAP lesions evaluation. The fibrocartilaginous labrum most often has a triangular structure, but it may change shape dynamically with traction from the capsule or glenohumeral ligaments (e.g., appear round or flattened). Regardless, if there is no high signal either at the labral–chondral junction or through the labrum, the labrum should be graded as normal. The sublabral sulcus (also referred to as a sublabral recess) and sublabral foramen are frequent anatomic variations, in which a segment of the labrum is not attached to the underlying glenoid. Typically a sublabral sulcus appears as a cleft of smooth, medially curved increased signal at the chondrolabral junction that does not extend posterior to the biceps anchor. The depth of the recess is variable, but typically less than 2 mm. Despite that, it must be emphasized that high signal of more than 3 mm on MRA extending anterior and posterior to the biceps anchor or laterally in the substance of the tendon is the hallmark of SLAP lesions (Figure 10).[14]
SLAP Lesion
Computer tomography scan (CT)
CT arthrogram is reserved for patients who presents contraindications to MRA.
Arthroscopic Diagnosis
When a superior labral tear is suspected preoperatively, the superior labrum is then carefully evaluated arthroscopically for injury. The arthroscopic diagnosis of a SLAP lesion can be based on 5 specific findings:
- Drive through sign
- Increase sublabral sulcus > 5 mm
- Bare sublabral footprint
- Displaceable biceps root
- Peel-back sign.
A drive through sign occurs, when while viewing through a posterior portal the arthroscope can be easily “driven” from the superior aspect of the glenohumeral joint to the inferior aspect (i.e. axillary recess) of the glenohumeral joint with minimal pressure. This is indicative of the overall laxity of the joint that may occur with SLAP lesions.
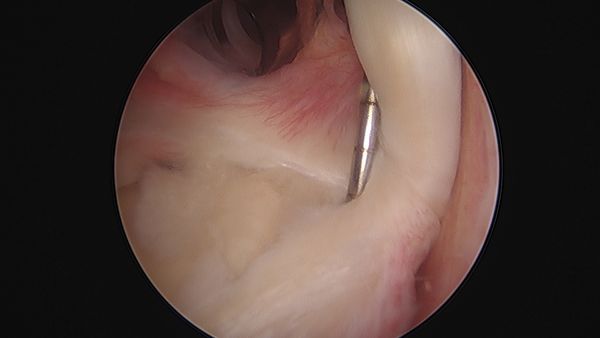
The normal sublabral sulcus ranges from approximately 3-5 mm and may increase with age. Therefore, if the sublabral sulcus is increased and associated with exposed bone (bare sublabral footprint), this is indicative of detachment of the superior labrum from the superior glenoid. It is particularly relevant, since the superior aspect of the glenoid under the labrum (the normal sublabral sulcus) is normally covered with articular cartilage (arthroscopic figure), a bare sublabral footprint with exposed bone (further supported by associated undersurface labral fraying) is again indicative of detachment of the superior labrum from the glenoid. When this detachment is significant, stability of the biceps root may be affected and the tendon may be easily translated medially and laterally with a probe (Figure 11).
Testing of SLAP Lesion
Finally, dynamic stability of the superior labrum and biceps root is evaluated by placing the arm in the functional throwing position of 90 degrees of abduction and full external rotation. In patients with an intact superior labrum the biceps root and superior labrum remain centered on the superior glenoid and the intra-articular portion of the biceps tendon merely changes its angular position to the superior labrum. However, in patients with tears of the superior labrum (particularly, if involving the posterior superior labrum), as the arm is brought into external rotation, the torsional force from the biceps tendon lifts the superior labrum off the glenoid and the labrum begins to “peel-back” off the glenoid and falls off medially. This is the "peel-back" sign that indicates an unstable superior labrum.
Although arthroscopy was considered the gold standard for SLAP diagnosis for a long time, interobserver and intraobserver variabilities have been demonstrated in the agreement on the diagnosis and treatment of SLAP lesions .[15]
Indications For Repair
In patients with an arthroscopic diagnosis of a SLAP lesion (i.e. satisfying the 5 criteria mentioned above) the decision to proceed with SLAP repair is largely based on the patients preoperative clinical suspicion. In patients with SLAP lesions with the primary complaint of instability and associated Bankart or reverse Bankart lesions, the SLAP lesion is universally repaired to provide a stable base for labral repair and enhance stability. Furthermore, in young patients (< 35 years), with throwing disability particularly in the absence of other major concomitant diagnoses, the SLAP lesion is repaired.
One should be particularly cognizant of the repair of a SLAP lesion diagnosed arthroscopically “en passant”, since repair may lead to persistent pain and stiffness postoperatively. In older patients (> 35 years), where pain is the primary complaint particularly in the presence of other concomitant diagnoses (i.e. rotator cuff tear), an alternative treatment of the SLAP lesion may be indicated (i.e. debridement , biceps tenodesis).[16][17]
A study reveals that at a mean age of 40 years neither labral repair nor biceps tenodesis had any significant clinical benefit over sham surgery for patients with SLAP II lesions.[18]
Treatment
Conservative treatment
The conservative treatment of initial symptomatic SLAP disease consists of cooling, anti-inflammatory drugs, cortisone glenohumeral injection, physical therapy and a rest period. Proprioceptive training is fundamental, especially after shoulder injuries, in order to prevent re-injury. An extensive physical therapy program may modify the scapulothoracic dyskinesis. Rotator cuff and periscapular strengthening exercises combined with a intra-articular corticosteroid injection provided satisfactory clinical outcomes in 85% of 30- to 45-year-old patients.[19]
In overhead athletes, special attention should be paid to correct repetitive and unbalanced movement. A retrospective case series demonstrated that the rate of return to prior performance level in professional baseball pitchers with SLAP lesions after non-operative treatment was 22%.[20][21]
The surgical indications remain unclear: 54% of the papers analyzed in a systematic review did not report the arthroscopic indications for repair of the SLAP lesion. They also described a wide variability in the current practice for the surgical treatment of SLAP lesions.[22]
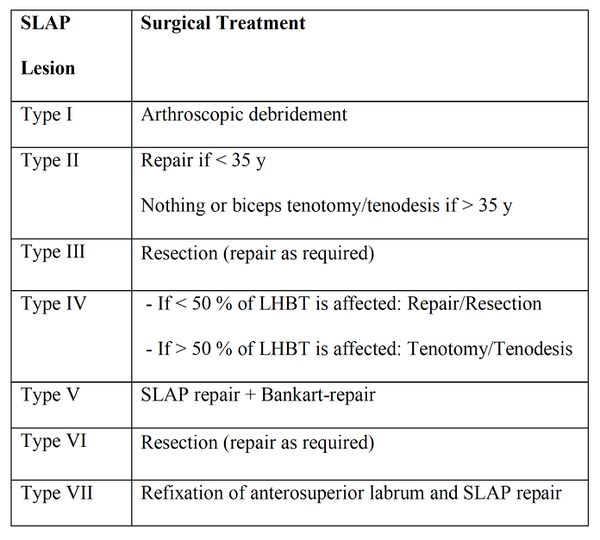
Labral/biceps tear or excessive labral mobility is commonly accepted as indication for repair. We suggest that if the non-operative therapy fails and symptoms persist preventing activities of daily living for longer than 6 months, operative treatment might be indicated. A surgical treatment algorithm for SLAP lesions is presented in Table 2.
Table: Suggestion for the treatment algorithm of SLAP lesions
Surgical technique
Different surgical techniques were described for arthroscopic SLAP repair. Various suture anchor placement and suture loop constructs were investigated without any clear differences for specific repair type. Currently, the technique most commonly used by experienced shoulder arthroscopists involves placement of one or more suture anchors in the superior glenoid, passage of the suture through the labrum and securing it by use of arthroscopic knots.
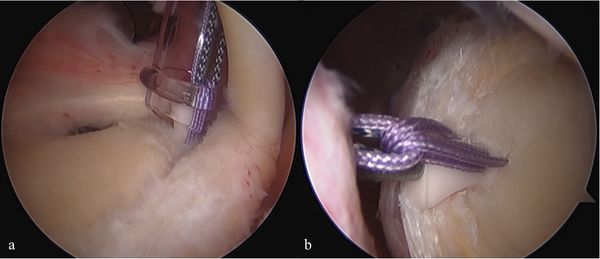
To appropriately place a suture anchor in the superior glenoid and to prevent iatrogenic injury to the glenoid articular cartilage it is fundamental to achieve a proper working-angle. We advocate of the use of a portal placed anterior to the acromion, entering the joint through the rotator interval. This decreases the risk of injury to the rotator cuff and works well for placement of anchors anterior to the biceps tendon (Figure 13A), but can result in an angle from anterior to posterior that makes it difficult to gain posterior anchors placed. When the tear extends more posteriorly to the posterosuperior quadrant, a second anchor is required. Due to the rounded shape of the superior glenoid, the anterosuperolateral portal usually does not provide the correct angle of approach to the posterosuperior glenoid. A separate portal, the Port of Wilmington portal, is required which is created approximately 1 cm anterior and 1 cm lateral to the posterolateral corner of the acromion. For posterior lesions, the suture anchor can be placed through the standard posterior portal (Figure 13B).
A portal placed lateral to the acromion has become popular, because this generally provides an appropriate angle for insertion of suture anchors. Placement of a portal lateral to the acromion needs a careful penetration of the rotator cuff to access the superior glenoid.
The most important endpoint of this surgery is the mechanical application of the labrum to the glenoid, restoration of joint function, such as biceps root mobility, elimination of the peel back, and restoration of tension in the posterior labrum and posterior inferior glenohumeral ligament.
The number of used anchors is known to be an important technical component. An inadequate attachment footprint on the glenoid does not generate adequate healing. Multiple fixation points achieved by using multiple individual anchors improve labral stability.[23]
Associated Spinoglenoid Cyst With Type II SLAP Repair
Most spinoglenoid cysts resolve after labral fixation without cyst decompression.[24]
Rehabilitation Protocol
Phase I (from surgery to 3-4 weeks after surgery)
Sling immobilization required for soft tissue healing avoiding range of motion with long lever arm shoulder flexion, as well as resisted supination or elbow flexion. Avoid excessive abduction and external rotation for 4 weeks. Gentle active range of motion for elbow and wrist. Cooling, anti-inflammatory drugs and a rest period may help the patient.
Phase II (4 to 8 weeks after surgery)
Capsular stretching is indicated in this phase. Patients were encouraged work with physiotherapist assistance. The goal is to recover full passive rotator cuff range of motion in a neutral position and full passive scapular motion. Control pain and inflammation with cooling, anti-inflammatory drugs and physical therapy.
Phase III (usually starting from 8 to 12 weeks after surgery)
Continue all strengthening activities increasing resistance and repetition. Physiotherapist assistance is indicated to improve upper extremity endurance, neuromuscular control and normalize arthrokinematics. Full passive and increasing active range of motion avoiding activities, where a higher risk exists for falling or outside forces to be applied to the arm.
Phase IV (usually starting from 12 to 16 weeks after surgery)
Continue eccentric strengthening of the rotator cuff and scapular musculature. Recover full passive and active range of motion until gradual return to sports specific functional training. Full return to throwing and contact sports occurs in 80-90% of athletes.[25][26]
References
- ↑ Cooper DE, Arnoczky SP, O'Brien SJ, Warren RF, DiCarlo E, Allen AA. Anatomy, histology, and vascularity of the glenoid labrum. An anatomical study. J Bone Joint Surg Am. 1992;74:46-52.
- ↑ Huber WP, Putz RV. Periarticular fiber system of the shoulder joint. Arthroscopy. 1997;13:680-91.
- ↑ Chang D, Mohana-Borges A, Borso M, Chung CB. SLAP lesions: Anatomy, clinical presentation, MR imaging diagnosis and characterization. Eur J Radiol 2008;68:72–87
- ↑ Kadi R, Milants A, Shahabpour M. Shoulder Anatomy and Normal Variants. J Belg Soc Radiol. 2017;101(S2):3.
- ↑ 5.0 5.1 5.2 Snyder SJ, Karzel RP, Pizzo WD, Ferkel RD, Friedman MJ. Arthroscopy classics. SLAP lesions of the shoulder. Arthroscopy. 2010;26:1117
- ↑ Morgan CD, Burkhart SS, Palmeri M, Gillespie M. Type II SLAP lesions: three subtypes and their relationships to superior instability and rotator cuff tears. Arthroscopy 1998;14:553-65.
- ↑ Kim TK, Queale WS, Cosgarea AJ, McFarland EG. Clinical features of the different types of SLAP lesions: An analysis of one hundred and thirty-nine cases. J Bone Joint Surg Am. 2003;85:66-71.
- ↑ Onyekwelu I, Khatib O, Zuckerman JD, Rokito AS, Kwon YW. The rising incidence of arthroscopic superior labrum anterior and posterior (SLAP) repairs. J Shoulder Elbow Surg. 2012;21:728-31.
- ↑ 9.0 9.1 Rokito SE, Myers KR, Ryu RK. SLAP lesions in the overhead athlete. Sports Med Arthrosc Rev. 2014;22:110-6.
- ↑ Zhang AL, Kreulen C, Ngo SS, Hame SL, Wang JC, Gamradt SC. Demographic trends in arthroscopic SLAP repair in the United States. Am J Sports Med. 2012;40:1144-7.
- ↑ Joo HO, Jae YK, Woo SK, Hyun SG, Ji HL: The evaluation of various physical examinations for the diagnosis of type II superior labrum anterior and posterior lesion. Am J Sports Med. 2008;36:353-9.
- ↑ Meserve BB1, Cleland JA, Boucher TR. A meta-analysis examining clinical test utility for assessing superior labral anterior posterior lesions. Am J Sports Med. 2009;37:2252-8.
- ↑ 13.0 13.1 Arirachakaran A, Boonard M, Chaijenkij K, Pituckanotai K, Prommahachai A, Kongtharvonskul J. A systematic review and meta-analysis of diagnostic test of MRA versus MRI for detection superior labrum anterior to posterior lesions type II-VII. Skeletal Radiol. 2017;46:149-60.
- ↑ Itoigawa Y., Itoi E. Anatomy of the capsulolabral complex and rotator interval related to glenohumeral instability. Knee Surg. Sports Traumatol. Arthrosc. 2016;24:343–9.
- ↑ Gobezie R, Zurakowski D, Lavery K, Millett PJ, Cole BJ, Warner JJP. Analysis of interobserver and intraobserver variability in the diagnosis and treatment of SLAP tears using the Snyder classification. Am J Sports Med. 2008;36:1373-9.
- ↑ Denard PJ, Lädermann A, Parsley BK, Burkhart SS. Arthroscopic biceps tenodesis compared with repair of isolated type II SLAP lesions in patients older than 35 years. Orthopedics. 2014;37:e292-7.
- ↑ Boileau P, Parratte S, Chuinard C, Roussanne Y, Shia D, Bicknell R. Arthroscopic Treatment of Isolated Type II SLAP Lesions: Biceps tenodesis as an alternative to reinsertion. Am J Sports Med 2009;37:929–36
- ↑ Schrøder CP, Skare Ø, Reikerås O, Mowinckel P, Brox JI. Sham surgery versus labral repair or biceps tenodesis for type II SLAP lesions of the shoulder: a three-armed randomised clinical trial. Br J Sports Med. 2017;51:1759-66.
- ↑ Shin SJ, Lee J, Jeon YS, Ko YW, Kim RG. Clinical outcomes of non-operative treatment for patients presenting SLAP lesions in diagnostic provocative tests and MR arthrography. Knee Surgery, Sport Traumatol Arthrosc 2017;25:3296–302.
- ↑ Brockmeyer M, Tompkins M, Kohn DM, Lorbach O. SLAP lesions: a treatment algorithm. Knee Surg Sports Traumatol Arthrosc. 2016;24:447-55.
- ↑ Fedoriw WW, Ramkumar P, McCulloch PC, Lintner DM, Referenciado M. Return to play after treatment of shoulder labral tears in baseball profesional players. Phys Sportsmed 2014;44:119–25.
- ↑ Kibler W Ben, Sciascia A. Current Practice for the Surgical Treatment of SLAP Lesions: A Systematic Review. Arthroscopy. 2016;32:669-83.
- ↑ Kim SJ, Kim SH, Lee SK, Lee JH, Chun Y. Footprint contact restoration between the biceps-labrum complex and the glenoid rim in SLAP repair: A comparative cadaveric study using pressure-sensitive film. Arthroscopy 2013;29:1005–11.
- ↑ Schroder CP, Skare O, Stiris M, Gjengedal E, Uppheim G, Brox JI. Treatment of labral tears with associated spinoglenoid cysts without cyst decompression. J Bone Joint Surg Am. 2008;90:523-30.
- ↑ Funk L, Snow M. SLAP tears of the glenoid labrum in contact athletes. Clin J Sport Med. 2007;17:1-4.
- ↑ Park H Bin, Lin SK, Yokota A, McFarland EG. Return to play for rotator cuff injuries and superior labrum anterior posterior (SLAP) lesions. Clin Sports Med. 2004;23:321-34.