Shoulder:Rotator Cuff Pathology/Thickness Rotator Cuff Tears/Traumatic versus degenerative tears
Contents
- 1 Bullet points
- 2 Key Words
- 3 Introduction
- 4 Natural phenomena
- 5 Criteria
- 6 Conclusion
- 7 References
Bullet points
- Accidental lesion and lesion assimilated to an accidental lesion are two legal concepts.
- They require expert medical knowledge to determine whether the lesion is of degenerative or traumatic nature.
- Minor degenerative disorders, symptomatic or asymptomatic depending on the individual, are frequent over age 30 and should no longer be taken into account in deciding whether the origin of a lesion was traumatic or degenerative.
- The prevalence of full-thickness degenerative lesions has significantly decreased over the last 15 years.
- Full-thickness and anterior lesions are often accidental in younger subjects.
- Demographic, anamnestic, clinical, radiographic and intraoperative data should be used to distinguish between degenerative and traumatic lesions.
- Traumatic rotator cuff tears need to be operated within 3 weeks in order to have the best functional outcomes
Key Words
Rotator Cuff Pathology; Full Thickness Rotator Cuff Tears; Traumatic; Degenerative.
Introduction
Traumatic lesion and lesion assimilated to a traumatic lesion are in some countries two legal concepts. The criteria allowing differentiation between degenerative lesions and lesions probably due to an accident sometimes lead to interminable legal quarrels between patients, the insured and insurance companies. Legal disputes are thus legion and risk delaying treatment, to the detriment of both patient and employer. The issue is medically critical, as rapid treatment of traumatic rotator-cuff lesions is the key to good functional outcome.[1][2][3][4][5][6][7] The best functional outcomes can be expected when patients are treated surgically within 3 weeks following traumatic rotator cuff tears, as presented by Gutman et al.[8]
The main difficulty is to distinguish between a traumatic rotator-cuff lesion, acute exacerbation of a pre-existing degenerative lesion, and simple painful or functional decompensation of a pre-existing degenerative lesion.[2] It is important to collate and distinguish objective and indisputable demographic, anamnestic, clinical and radiographic rotator-cuff lesion data (e.g., fatty infiltration) as a basis to decide whether in a given case the tear was traumatic (or assimilated) or more likely of degenerative or disease-specific nature. It is thus a question of defining the clinical and paraclinical data that formally confirm or exclude accidental status. A single risk factor, such as smoking,[9][10] hypercholesterolemia,[11] alcohol abuse,[12] high blood pressure,[13] hyperthyroidism,[14] critical shoulder angle,[15][16] or morphology of the greater tuberosity[17] is not necessarily a criterion.
Natural phenomena
Minor degenerative disorders, which may be symptomatic or asymptomatic depending on the individual, are frequent over 30 years old[18][19] and should probably no longer be taken into account in deciding whether a given lesion is degenerative or accidental. An ultrasound study of 51 asymptomatic patients aged 40 to 70 years reported abnormalities such as tendinosis (65%), acromioclavicular osteoarthritis (65%), labral pathology (14%) and partial tear of the bursa side of the supraspinatus tendon (22%).[2] The supraspinatus tendon insertion on the greater tuberosity may show degeneration that is probably multifactorial: vascular,[20] mechanical,[21] morphologic,[22][23] and genetic.[24]
The prevalence of full-thickness rotator-cuff tear in the population under age 70 who has never shown symptoms is at most 15%.[2][25]
Criteria
Demographic criteria
Several studies have demonstrated that the prevalence of degenerative full-thickness tear is not as important as previously thought (Table 1).
| 20–30 y | 30–40 y | 40–50 y | 50–60 y | 60–70 y | 70–80 y | >80 y | |
| Tempelhof et al.[26] | 13% | 20% | 31% | 51% | |||
| Abate et al.[27] | 25% | 25% | |||||
| Fehringer et al.[28] | 22% | 22% | |||||
| Moosmayer et al.[29] | 2,1% | 5,7% | 15% | ||||
| Yamamoto et al.[25] | 0% | 0% | 0% | 10,7% | 15,2% | 26,5% | 36,8% |
| Liem et al.[30] | 0% | 0% | 0% | 0% | 13% | 37.5% | 0% |
Table 1: Prevalence of degenerative full-thickness tear
In an ultrasound study of asymptomatic subjects over 65 years old, Abate et al. reported the prevalence of rotator-cuff lesions:[27] only 3.1% of non-diabetic patients had partial or full thickness tears of less than 1 cm, and 7.8% had tears greater than 1 cm. In a study of 200 shoulders in 100 patients with a mean age of 71.4 years (range of 65-87 years), Fehringer et al. found 22% prevalence of full-thickness rotator-cuff lesions in patients consulting for lower-limb issues, whether the shoulder was symptomatic or not.[28] Another ultrasound and magnetic resonance imaging (MRI) assessment of 420 asymptomatic volunteers found a prevalence of full-thickness rotator cuff tear of 2%, 6% and 15% in the 50-59, 60-69 and 70-79 year-old age-groups respectively,[29] with location in the supraspinatus tendon in 78% of cases. In a similar study of 664 volunteers in a single village, prevalence of full-thickness tear was 22.1%:[25] 0% between 20 and 49 years of age, 10.7% for subjects in their 50s, 15.2% in the 60s, 26.5% in the 70s and 36.6% in over-79 year-olds; only 34.7% of these lesions were symptomatic. Liem et al. reported no rotator-cuff lesions in a control group of 55 under 60 years old.[30]
In summary, lesions are rarely full-thickness before the age of 60 (in fewer than 10% of cases even in the elderly), and involve the supraspinatus tendon in 85% of cases. Between 70 and 79 years of age, 74-89% of subjects have a functional rotator cuff. Traumatic tears concern younger subjects, with a mean age of 54 years.[5] A traumatic event was recorded in 79.2% of cases (57/72 shoulders) in a study of full-thickness cuff tear in subjects under 50 years old.[31]
Clinical criteria
Immediate impairment of active flexion or external rotation or onset of pseudoparalytic shoulder (loss of active anterior forward flexion) due to rotator-cuff tear are typical consequences of a trauma.[2][32][33][34][35] Berhouet et al. reported on 112 patients under 65 year old patients with rotator-cuff lesions. More than half of them had clearly been involved in an accident,[34] and all these patients showed loss of forward flexion or external rotation. Denard et al. prospectively studied 58 patients with pseudoparetic shoulder and rotator cuff tear;[35] 78% of the cases (45 out of 58) involved a trauma. There is thus a high rate of traumatic events associated with acute loss of function. Loew reported severe pain after traumatic rotator-cuff injury, subsiding after 3 days, which may account for delayed consultation and treatment.[32][33]
Factorial criteria
Only 5 studies reported the mechanism of traumatic rotator cuff lesions.[1][36][37][38][39] This mainly involves falling onto the arm in extension.[5] Other associated actions causing injury comprise external rotation against resistance, violent traction while trying to avoid a fall or lifting a heavy weight, or shoulder dislocation. However, the mechanism is usually unclear, especially in road accidents. The following actions should be considered:[32][33]
- Significant trauma with violent passive backward and inward movement of the arm, or arm stabilized by muscle action: for example, trying to avoid a fall from scaffolding or on stairs.
- Shoulder dislocation causes full-thickness cuff tear in 41% of cases in 40-to-55 year-olds, in 71% in 56-to-70 year-olds, and systematically in older subjects.[40]
- Suddenly hanging with the arm in suspension bearing full body-weight.
- Violent passive traction in adduction, antepulsion or abduction, as in wrenching the arm or trying to avoid a fall with arms outstretched.
- Axial impact during a fall on the elbow or hand.
- Direct shock to the shoulder without necessarily involving the arm in extension can also cause full-thickness tear.
Radiologic criteria
Correct analysis of assessment comprising conventional X-ray, ultrasound and magnetic resonance imaging (MRI) or computed tomography (CT) is often decisive and, in the light of present knowledge, can distinguish between degenerative and accidental lesions.
Conventional radiologic criteria
Acromion morphology and acromioclavicular osteoarthritis
Whether acromion morphology is a risk factor for rotator-cuff lesion is controversial. Acromion morphology according to Bigliani,[41] acromial slope in the frontal and parasagittal planes, lateral protrusion[42] and critical shoulder angle are debated factors.[15][16] Anterior coraco-acromial ligament spur,[43] presence of an os acromiale[44] and acromioclavicular arthropathy[45] do not correlate with rotator-cuff lesion; the only clear association is with acromial acetabulization.
Proximal humeral remodeling
Subchondral sclerosis and greater tuberosity subchondral cysts do not seem to be signs of chronic rotator-cuff lesion, having wide interobserver variability and poor predictive value.[46][47] They are thus not reliable signs of chronic or degenerative lesion, and seem to be related to age.[48] Chronic partial or retracted cuff lesions are associated with major remodeling of the greater tuberosity in the form of “femoralization” and osteopenia.[21][49][50][51] Localized greater tuberosity osteopenia on AP X-ray is the bone response to lack of mechanical stress (Wolff’s law).[52]
Acromio-humeral distance
Acromio-humeral distance <7 mm on anteroposterior shoulder view is a sign of chronic rotator-cuff tear.[53][54] Saupe et al. correlated this 7 mm threshold with computed tomography (CT)-arthrography evidence of lesion, and found full-thickness supraspinatus tear in 90% of cases, infraspinatus tear in 67% and subscapularis tear in 47%.[54] Distance <7 mm generally corresponds to a massive tear of several months’ progression, associated with altered muscle trophicity.[53][54]
Magnetic resonance imaging (MRI) and computed tomography (CT) criteria
The only irrefutable signs of accidental lesion are fractures and stigmata of glenohumeral or acromioclavicular dislocation.[55] Magnetic resonance imaging (MRI) and, to a lesser extent, computed tomography (CT) are now contributive to confirming or ruling out accidental etiology. Above all, they can rule out occult fracture, notably of the greater tuberosity.
Rotator-cuff muscle atrophy
Supraspinatus atrophy is assessed via the tangent sign.[56] A positive tangent sign is risk factors for incomplete rotator cuff repair repair.[57]
Rotator-cuff fatty infiltration
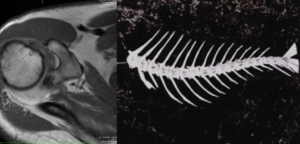
Magnetic resonance imaging (MRI)[58] and computed tomography (CT)[59] quantify fatty infiltration in the rotator-cuff muscles. This quantification is essential, as initial fatty infiltration exceeding grade 2 generally contraindicates repair surgery, because of a very high risk of healing failure. It is thus a decisive prognostic factor for clinical and radiological outcome.[60] For the supraspinatus muscle, it is more reliably assessed in the axial plane.[61] The fish backbone sign also indicates a chronic lesion (Figure 1).[61]
Fatty infiltration has several potential origines such as age or rotator cuff lesion.
- Fatty infiltration of rotator cuff muscles increased naturally with age, with a significant acceleration after 40 years. A fatty infiltration graded 2, a common threshold for management decision, is commonly found in those aging patients with intact cuff on computed tomography (CT) arthrography.[62] A fatty infiltration graded 2 or below is thus not always associated with a rotator cuff lesion.
- Fatty infiltration seem to appear quickly after a rotator cuff lesion, as soon as 3 weeks in animal models.[63][64] In humans, significant fatty infiltration is observed only after 6 months or if there is no traumatic etiology.[34] In both traumatic and non-traumatic cases, grade 2 fatty infiltration sets in at 3, 2.5 and 2.5 years after symptom onset in the supraspinatus, infraspinatus and subscapularis muscles, respectively; progression to grades 3 and 4 takes respectively 5, 4 and 3 years (Table 2).[65][66] Isolated supraspinatus lesions showed no significant fatty infiltration at 4 years’ follow-up.[67] In contrast, massive lesions become irreparable after the same period of time.[68]
| Time to onset (months) | Supraspinatus fatty infiltration | Infraspinatus fatty infiltration | Subsacapularis fatty infiltration | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Minimal | Intermediate | Severe | Minimal | Intermediate | Severe | Minimal | Intermediate | Severe | |
| Overall series | 24 | 46 | 70 | 26 | 44 | 67 | 24 | 34 | 46 |
| Traumatic onset | 19 | 35 | 58 | 19 | 31 | 46 | 17 | 31 | 39 |
| Progressive onset | 29 | 54 | 84 | 33 | 56 | 84 | 33 | 36 | 55 |
Table 2: Average time to onset of different fatty infiltration stages assessed in overall series and traumatic versus progressive onset.
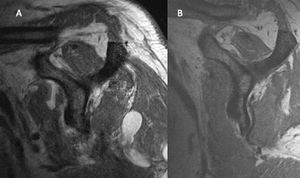
According to Goutallier,[59] significant fatty infiltration (grade 3 or 4, generally contraindicating repair) at the time of the accident probably involves decompensation or acute extension of a pre-existing lesion. Severe fatty infiltration may, however, develop within months of accidental massive lesion, particularly if the anterior rotator cuff is involved (Figure 2).
Bone and muscle edema
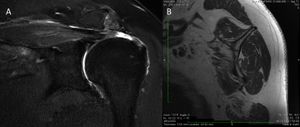
Greater tuberosity edema used to be thought of as being associated with full-thickness rotator-cuff tear,[69] but this was not confirmed in a more recent study.[55] Screening for muscle edema, on the other hand, is crucial. Except in real involvement of the muscle-tendon junction,[70] rare denervation phenomena as found in suprascapular nerve compression (<2%)[71] or Parsonage-Turner syndrome and other infrequent entities,[72] muscle edema is associated with acute retraction and indicates accidental etiology (Figure 3).[55] Onset is within days, unlike neurologic edema, where onset is a matter of weeks.
Changes in subacromial and subdeltoid bursa
Fluid or hematoma in the bursa is more frequently found in acute than chronic lesions, and is generally associated with lesions of the tendon rather than of the tendon-bone junction (mid-substance tear). Blood signal following an accident is a sign of traumatic rotator-cuff lesion.[74]
Location and type of tendon lesion
Location of the lesion is also an important factor. In the frontal plane, traumatic lesions generally involve the tendon itself.[74] Medial tendon retraction according to Patte[75] (Table) then develops,[69] generally with slow progression. Braune et al. found no retracted tendons in the glenoid or beyond 12 weeks after trauma.[76] However, some cases of grade 3 retraction at the glenoid without fatty infiltration may be found during the weeks following a trauma, suggesting acute massive lesions with severe muscle and tendon retraction. In the sagittal plane, subscapularis tendon lesions are typical of accidents.[3][36][77] Moreover, 80% of asymptomatic lesions involve the supraspinatus tendon.[29] Anterior or posterior extension in a previously asymptomatic patient suggests a traumatic etiology.
Intraoperative criteria
Lesion type alone may not be a sufficient criteria to determine a traumatic or non-traumatic etiology.[76] The most significant criteria for traumatic origin are hemarthrosis, tendon remnant on the greater tuberosity, frayed and bleeding tendon edge, and subscapularis involvement.[73][76]
Conclusion
Rotator-cuff tears are most often degenerative but some may nevertheless be caused or aggravated by a traumatic event. It is not recommended to apply just a single criterion, such as age, to determine whether a causal relation is above or below the threshold of likelihood. The field of application of the concept of causality (no accident, no injury) is deliberately wide; ruling it out requires an exhaustive argumentation using all of the criteria defined above.
References
- ↑ 1.0 1.1 Bassett RW, Cofield RH. Acute tears of the rotator cuff. The timing of surgical repair. Clin Orthop Relat Res. 1983;(175):18-24.
- ↑ 2.0 2.1 2.2 2.3 2.4 Lähteenmäki HE, Virolainen P, Hiltunen A, Heikkilä J, Nelimarkka OI. Results of early operative treatment of rotator cuff tears with acute symptoms. J Shoulder Elbow Surg. 2006;15:148-53.
- ↑ 3.0 3.1 Krishnan SG, Harkins DC, Schiffern SC, Pennington SD, Burkhead WZ. Arthroscopic repair of full-thickness tears of the rotator cuff in patients younger than 40 years. Arthroscopy. 2008;24:324-8.
- ↑ Petersen SA, Murphy TP. The timing of rotator cuff repair for the restoration of function. J Shoulder Elbow Surg. 2011;20:62-8.
- ↑ 5.0 5.1 5.2 Mall NA, Lee AS, Chahal J, Sherman SL, Romeo AA, Verma NN, Cole BJ. An evidenced-based examination of the epidemiology and outcomes of traumatic rotator cuff tears. Arthroscopy. 2013;29:366-76.
- ↑ Duncan NS, Booker SJ, Gooding BW, Geoghegan J, Wallace WA, Manning PA. Surgery within 6 months of an acute rotator cuff tear significantly improves outcome. J Shoulder Elbow Surg. 2015;24:1876-80.
- ↑ Tan M, Lam PH, Le BT, Murrell GA. Trauma versus no trauma: an analysis of the effect of tear mechanism on tendon healing in 1300 consecutive patients after arthroscopic rotator cuff repair. J Shoulder Elbow Surg. 2016;25:12-21.
- ↑ Gutman MJ, Joyce CD, Patel MS, Kirsch JM, Gutman BS, Abboud JA, Namdari S, Ramsey ML. Early repair of traumatic rotator cuff tears improves functional outcomes. J Shoulder Elbow Surg. 2021:S1058-2746(21)00331-1.
- ↑ Bishop JY, Santiago-Torres JE, Rimmke N, Flanigan DC. Smoking Predisposes to Rotator Cuff Pathology and Shoulder Dysfunction: A Systematic Review. Arthroscopy. 2015;31:1598-605.
- ↑ Santiago-Torres J, Flanigan DC, Butler RB, Bishop JY. The effect of smoking on rotator cuff and glenoid labrum surgery: a systematic review. Am J Sports Med. 2015;43:745-51.
- ↑ Chung SW, Park H, Kwon J, Choe GY, Kim SH, Oh JH. Effect of Hypercholesterolemia on Fatty Infiltration and Quality of Tendon-to-Bone Healing in a Rabbit Model of a Chronic Rotator Cuff Tear: Electrophysiological, Biomechanical, and Histological Analyses. Am J Sports Med. 2016;44:1153-64.
- ↑ Passaretti D, Candela V, Venditto T, Giannicola G, Gumina S. Association between alcohol consumption and rotator cuff tear. Acta Orthop. 2016;87:165-8.
- ↑ Gumina S, Arceri V, Carbone S, Albino P, Passaretti D, Campagna V, Fagnani C, Postacchini F. The association between arterial hypertension and rotator cuff tear: the influence on rotator cuff tear sizes. J Shoulder Elbow Surg. 2013;22:229-32.
- ↑ Oliva F, Osti L, Padulo J, Maffulli N. Epidemiology of the rotator cuff tears: a new incidence related to thyroid disease.Muscles Ligaments Tendons J. 2014;4:309-14.
- ↑ 15.0 15.1 Balke M, Schmidt C, Dedy N, Banerjee M, Bouillon B, Liem D. Correlation of acromial morphology with impingement syndrome and rotator cuff tears. Acta Orthop. 2013;84:178-83.
- ↑ 16.0 16.1 Moor BK, Wieser K, Slankamenac K, Gerber C, Bouaicha S. Relationship of individual scapular anatomy and degenerative rotator cuff tears. J Shoulder Elbow Surg. 2014;23:536-41.
- ↑ Cunningham G, Nicodème-Paulin E, Smith MM, Holzer N, Cass B, Young AA. The greater tuberosity angle: a new predictor for rotator cuff tear. J Shoulder Elbow Surg. 2018;27:1415-1421.
- ↑ Girish G, Lobo LG, Jacobson JA, Morag Y, Miller B, Jamadar DA. Ultrasound of the shoulder: asymptomatic findings in men. AJR Am J Roentgenol. 2011;197:W713-9.
- ↑ Teunis T, Lubberts B, Reilly BT, Ring D. A systematic review and pooled analysis of the prevalence of rotator cuff disease with increasing age. J Shoulder Elbow Surg. 2014;23:1913-1921.
- ↑ Adler RS, Fealy S, Rudzki JR, Kadrmas W, Verma NN, Pearle A, Lyman S, Warren RF. Rotator cuff in asymptomatic volunteers: contrast-enhanced US depiction of intratendinous and peritendinous vascularity. Radiology. 2008;248:954-61.
- ↑ 21.0 21.1 Neer CS 2nd. Anterior acromioplasty for the chronic impingement syndrome in the shoulder: a preliminary report. J Bone Joint Surg Am. 1972;54:41-50.
- ↑ Moor BK, Bouaicha S, Rothenfluh DA, Sukthankar A, Gerber C. Is there an association between the individual anatomy of the scapula and the development of rotator cuff tears or osteoarthritis of the glenohumeral joint?: A radiological study of the critical shoulder angle. Bone Joint J. 2013;95-B(7):935-41.
- ↑ Moor BK, Röthlisberger M, Müller DA, Zumstein MA, Bouaicha S, Ehlinger M, Gerber C. Age, trauma and the critical shoulder angle accurately predict supraspinatus tendon tears. Orthop Traumatol Surg Res. 2014;100:489-94.
- ↑ Gwilym SE, Watkins B, Cooper CD, Harvie P, Auplish S, Pollard TC, Rees JL, Carr AJ. Genetic influences in the progression of tears of the rotator cuff. J Bone Joint Surg Br. 2009;91:915-7.
- ↑ 25.0 25.1 25.2 Yamamoto A, Takagishi K, Osawa T, Yanagawa T, Nakajima D, Shitara H, Kobayashi T. Prevalence and risk factors of a rotator cuff tear in the general population. J Shoulder Elbow Surg. 2010;19:116-20.
- ↑ Tempelhof S, Rupp S, Seil R. Age-related prevalence of rotator cuff tears in asymptomatic shoulders. J Shoulder Elbow Surg. 1999;8:296-9.
- ↑ 27.0 27.1 Abate M, Schiavone C, Salini V. Sonographic evaluation of the shoulder in asymptomatic elderly subjects with diabetes. BMC Musculoskelet Disord. 2010;7:278.
- ↑ 28.0 28.1 Fehringer EV, Sun J, VanOeveren LS, Keller BK, Matsen FA 3rd. Full-thickness rotator cuff tear prevalence and correlation with function and co-morbidities in patients sixty-five years and older.J Shoulder Elbow Surg. 2008;17:881-5.
- ↑ 29.0 29.1 29.2 Moosmayer S, Smith HJ, Tariq R, Larmo A. Prevalence and characteristics of asymptomatic tears of the rotator cuff: an ultrasonographic and clinical study. J Bone Joint Surg Br. 2009;91:196-200.
- ↑ 30.0 30.1 Liem D, Buschmann VE, Schmidt C, Gosheger G, Vogler T, Schulte TL, Balke M. The prevalence of rotator cuff tears: is the contralateral shoulder at risk? Am J Sports Med. 2014;42:826-30.
- ↑ Lin YP, Huang TF, Hung SC, Ma HL, Liu CL. Rotator cuff tears in patients younger than 50 years of age. Acta Orthop Belg. 2012;78:592-6.
- ↑ 32.0 32.1 32.2 Loew M. [Traumatic development of rotator cuff lesion. Scientific principles and consequences for expert assessment]. Orthopade. 2000;29:881-7.
- ↑ 33.0 33.1 33.2 Loew M, Habermeyer P, Wiedemann E, Rickert M, Gohlke F. [Recommendations for diagnosis and expert assessment of traumatic rotator cuff lesions]. Unfallchirurg. 2000;103:417-26.
- ↑ 34.0 34.1 34.2 Berhouet J, Collin P, Benkalfate T, Le Du C, Duparc F, Courage O, Favard L, Société d'Orthopédie de l'Ouest. Massive Rotator Cuff Tears in Patients Younger Than 65 Years. Epidemiology and Characteristics. Orthop Traumatol Surg Res. 2009;95(4 Suppl 1):S13-8
- ↑ 35.0 35.1 Denard PJ, Lädermann A, Brady PC, Narbona P, Adams CR, Arrigoni P, Huberty D, Zlatkin MB, Sanders TG, Burkhart SS. Pseudoparalysis From a Massive Rotator Cuff Tear Is Reliably Reversed With an Arthroscopic Rotator Cuff Repair in Patients Without Preoperative Glenohumeral Arthritis. Am J Sports Med. 2015;43(10):2373-8
- ↑ 36.0 36.1 Gerber C, Hersche O, Farron A. Isolated Rupture of the Subscapularis Tendon. Bone Joint Surg Am. 1996;78:1015-23.
- ↑ Ide J, Tokiyoshi A, Hirose J, Mizuta H. Arthroscopic repair of traumatic combined rotator cuff tears involving the subscapularis tendon. J Bone Joint Surg Am. 2007;89:2378-88.
- ↑ Namdari S, Henn RF 3rd, Green A. Traumatic anterosuperior rotator cuff tears: the outcome of open surgical repair. J Bone Joint Surg Am. 2008;90:1906-13.
- ↑ Bjornsson H, Norlin R, Knutsson A, Adolfsson L. Fewer rotator cuff tears fifteen years after arthroscopic subacromial decompression. J Shoulder Elbow Surg 2010;19:111-115.
- ↑ Simank HG, Dauer G, Schneider S, Loew M. Incidence of rotator cuff tears in shoulder dislocations and results of therapy in older patients. Arch Orthop Trauma Surg 2006;126:235-240.
- ↑ Bigliani LU, Ticker JB, Flatow EL, Soslowsky LJ, Mow VC. [Relationship of acromial architecture and diseases of the rotator cuff]. Der Orthopade 1991;20:302-309.
- ↑ Nyffeler RW, Werner CM, Sukthankar A, Schmid MR, Gerber C. Association of a large lateral extension of the acromion with rotator cuff tears. J Bone Joint Surg Am. 2006;88:800-805.
- ↑ Gill TJ, McIrvin E, Kocher MS, Homa K, Mair SD, Hawkins RJ. The relative importance of acromial morphology and age with respect to rotator cuff pathology. J Shoulder Elbow Surg. 2002;11:327-330.
- ↑ Ouellette H, Thomas BJ, Kassarjian A, Fritz B, Tétreault P, Palmer WE, Torriani M. Re-examining the association of os acromiale with supraspinatus and infraspinatus tears. Skeletal radiology. 2007;36:835-9.
- ↑ Needell SD, Zlatkin MB, Sher JS, Murphy BJ, Uribe JW. MR imaging of the rotator cuff: peritendinous and bone abnormalities in an asymptomatic population. AJR. American journal of roentgenology. 1996;166:863-867.
- ↑ Huang LF, Rubin DA, Britton CA. Greater tuberosity changes as revealed by radiography: lack of clinical usefulness in patients with rotator cuff disease. AJR. American journal of roentgenology. 1999;172:1381-1388
- ↑ Williams M, Lambert RG, Jhangri GS, Grace M, Zelazo J, Wong B, Dhillon SS. Humeral head cysts and rotator cuff tears: an MR arthrographic study. Skeletal radiology. 2006;35:909-914
- ↑ Suluova F, Kanatli U, Ozturk BY, Esen E, Bolukbasi S. Humeral Head Cysts: Association With Rotator Cuff Tears and Age. J Orthop Surg Traumatol 2014;24:733-9.
- ↑ Neer CS, 2nd, Craig EV, Fukuda H. Cuff-tear arthropathy. J Bone Joint Surg Am. 1983;65:1232-1244.
- ↑ Jiang Y, Zhao J, van Holsbeeck MT, Flynn MJ, Ouyang X, Genant HK. Trabecular microstructure and surface changes in the greater tuberosity in rotator cuff tears. Skeletal radiology 2002;31:522-528.
- ↑ Meyer DC, Fucentese SF, Koller B, Gerber C. Association of osteopenia of the humeral head with full-thickness rotator cuff tears. J Shoulder Elbow Surg 2004;13:333-7.
- ↑ Wolff J. [Das Gesetz der Transformation der Knochen]. Berlin: Hirschwald Verlag; 1892
- ↑ 53.0 53.1 Nove-Josserand L, Edwards TB, O'Connor DP, Walch G. The acromiohumeral and coracohumeral intervals are abnormal in rotator cuff tears with muscular fatty degeneration. Clin Orthop Relat Res. 2005:90-96.
- ↑ 54.0 54.1 54.2 Saupe N, Pfirrmann CW, Schmid MR, Jost B, Werner CM, Zanetti M. Association between rotator cuff abnormalities and reduced acromiohumeral distance. AJR. American journal of roentgenology. 2006;187:376-382.
- ↑ 55.0 55.1 55.2 Loew M, Magosch P, Lichtenberg S, Habermeyer P, Porschke F. How to discriminate between acute traumatic and chronic degenerative rotator cuff lesions: an analysis of specific criteria on radiography and magnetic resonance imaging. J Shoulder Elbow Surg. 2015;24:1685-1693.
- ↑ Zanetti M, Weishaupt D, Jost B, Hodler J. MR abnormalities in patients suspected of having acute traumatic rotator cuff tears: Greater tuberosity fractures and subscapularis tendon tears are common. Radiology. 1998;209P:343-343.
- ↑ Sheean AJ, Hartzler RU, Denard PJ, Lädermann A, Sanders TG, Zlatkin MB, Burkhart SS. Preoperative Radiographic Risk Factors for Incomplete Arthroscopic Supraspinatus Tendon Repair in Massive Rotator Cuff Tears. Arthroscopy. 2018;34:1121-7.
- ↑ Fuchs B, Weishaupt D, Zanetti M, Hodler J, Gerber C. Fatty degeneration of the muscles of the rotator cuff: assessment by computed tomography versus magnetic resonance imaging. J Shoulder Elbow Surg. 1999;8:599-605.
- ↑ 59.0 59.1 Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC. Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res. 1994:78-83.
- ↑ Zumstein MA, Jost B, Hempel J, Hodler J, Gerber C. The clinical and structural long-term results of open repair of massive tears of the rotator cuff. J Bone Joint Surg Am. 2008;90:2423-2431.
- ↑ 61.0 61.1 Williams MD, Lädermann A, Melis B, Barthelemy R, Walch G. Fatty infiltration of the supraspinatus: a reliability study. J Shoulder Elbow Surg. 2009;18:581-587.
- ↑ Gueniche J, Bierry G. Rotator cuff muscles fatty infiltration increases with age: retrospective review of 210 patients with intact cuff on computed tomography arthrography. J Shoulder Elbow Surg. 2019;28:617-624.
- ↑ Liu X, Manzano G, Kim HT, Feeley BT. A rat model of massive rotator cuff tears. J Orthop Res. 2011;29:588-595.
- ↑ Mallon WJ, Wilson RJ, Basamania CJ. The association of suprascapular neuropathy with massive rotator cuff tears: a preliminary report. J Shoulder Elbow Surg. 2006;15:395-398.
- ↑ Melis B, Nemoz C, Walch G. Muscle fatty infiltration in rotator cuff tears: descriptive analysis of 1688 cases. Orthop Traumatol Surg Res. 2009;95:319-24.
- ↑ Melis B, DeFranco MJ, Chuinard C, Walch G. Natural history of fatty infiltration and atrophy of the supraspinatus muscle in rotator cuff tears. Clin Orthop Relat Res. 2010;468:1498-1505.
- ↑ Fucentese SF, von Roll AL, Pfirrmann CW, Gerber C, Jost B. Evolution of nonoperatively treated symptomatic isolated full-thickness supraspinatus tears. J Bone Joint Surg Am. 2012;94:801-8.
- ↑ Zingg PO, Jost B, Sukthankar A, Buhler M, Pfirrmann CW, Gerber C. Clinical and structural outcomes of nonoperative management of massive rotator cuff tears. J Bone Joint Surg Am. 2007;89:1928-1934.
- ↑ 69.0 69.1 McCauley TR, Disler DG, Tam MK. Bone marrow edema in the greater tuberosity of the humerus at MR imaging: association with rotator cuff tears and traumatic injury. Magn Reson Imaging. 2000;18:979-984.
- ↑ Lädermann A, Christophe FK, Denard PJ, Walch G. Supraspinatus rupture at the musclotendinous junction: an uncommonly recognized phenomenon. J Shoulder Elbow Surg. 2012;21:72-76.
- ↑ Collin P, Treseder T, Lädermann A, Benkalfate T, Mourtada R, Courage O, Favard L. Neuropathy of the suprascapular nerve and massive rotator cuff tears: a prospective electromyographic study. J Shoulder Elbow Surg. 2014;23:28-34.
- ↑ May DA, Disler DG, Jones EA, Balkissoon AA, Manaster BJ. Abnormal signal intensity in skeletal muscle at MR imaging: patterns, pearls, and pitfalls. Radiographics 2000;20:S295-315.
- ↑ 73.0 73.1 Loew M, Porschke FB, Riedmann S, Magosch P, Lichtenberg S. Zur Unterscheidung zwischen traumatischer und degenerativer Rotatorenmanschettenruptur –eine klinische und radiologische Untersuchung. Obere Extremität 2014;9:209–214.
- ↑ 74.0 74.1 Teefey SA, Middleton WD, Bauer GS, Hildebolt CF, Yamaguchi K. Sonographic differences in the appearance of acute and chronic full-thickness rotator cuff tears. J Ultrasound Med 2000;19:377-378
- ↑ Patte D. Classification of rotator cuff lesions. Clin Orthop Relat Res. 1990:81-86
- ↑ 76.0 76.1 76.2 Braune C, Gramlich H, Habermeyer P. Intraoperative shape of rotator cuff tears in traumatic and non traumatic cases. Der Unfallchirurg. 2000;103:462-467.
- ↑ Bjornsson HC, Norlin R, Johansson K, Adolfsson LE. The influence of age, delay of repair, and tendon involvement in acute rotator cuff tears: structural and clinical outcomes after repair of 42 shoulders. Acta Orthop. 2011;82:187-192